Pelvic Health Physiotherapy in Pregnancy and Beyond: Practical Guidance, Pregnancy to Postpartum
John Velasquez • March 2, 2026
The silent load your pelvic floor carries every day
Before we map your plan from pregnancy to postpartum, let’s make the invisible work visible. In Canadian research, about 1 in 3 people leak urine after birth—common, not normal. Picture it: a cough on the streetcar, a sneeze in a meeting, a quick run for the TTC turnstile. Each moment loads your pelvic floor, and those small leaks chip away at confidence.
Add pregnancy hormones, a growing belly, and long desk hours, and the pressure climbs. Studies report pelvic girdle or tailbone pain in about 1 in 5 during pregnancy, and many experience painful sex in the early months postpartum. Stress matters too—it can keep those muscles clenched. The good news? With targeted strategies and coaching, most symptoms ease quickly. We help you start safely, then build strength that lasts.
✨ Myth Buster
Leaking when you cough or sneeze isn’t normal—it’s treatable. Pain with intercourse isn’t normal—you deserve comfort. Pelvic heaviness or a “dragging” feeling isn’t normal—reach out.
What your pelvic floor does—and why pregnancy changes it
If leaking, pain with sex, or a dragging heaviness sound familiar, you’re not broken. Your pelvic floor is a hammock of muscles and connective tissue at the base of your pelvis, holding up your bladder, uterus, and bowel. It works with your diaphragm (your main breathing muscle), deep core, and hips to control pressure. Its jobs are support, bladder and bowel control, sexual function, and stability for your back and pelvis. Tight isn’t the same as strong; coordination matters.
Think of it like a responsive trampoline that moves with you. It should relax to let you pee and poop, lengthen for penetration, recoil when you cough or lift, and generate force when you run or jump. Daily life tests it: lifting groceries, chasing the streetcar, a Pilates teaser, even a deep laugh. When timing is off, leaks, heaviness, or pain can show up. We help you retrain the timing.
Pregnancy shifts the load and the rules. Relaxin (a hormone that softens ligaments) makes joints looser, while a growing uterus adds downward pressure. Posture changes and shorter breaths can increase pressure on that hammock. Vaginal birth stretches tissues; tearing or stitches can change sensation and timing. A Cesarean birth (abdominal surgery) doesn’t bypass the system—it alters your core pressure and scar mobility. Longer pushing, forceps, or vacuum can add strain. Put together, coordination can wobble. That’s why symptoms appear—and why targeted care helps.
How pelvic floor symptoms actually show up
These signs can come from muscles that are too tight, too weak, or not well coordinated—and they affect more than your bladder. Notice what shows up for you; it helps us tailor care.
- Leakage with coughing, sneezing, laughing, exercise
- Pelvic heaviness, dragging, or prolapse sensations
- Constipation, incomplete emptying, or fecal smearing
- Pain with intercourse or pelvic exams
- Pubic symphysis or tailbone pain (sitting, rolling, walking)
- Low back, hip, or groin pain linked to pelvic instability
- Abdominal doming/coning or diastasis recti signs
- Urinary urgency/frequency or nighttime urination
Why 'just do Kegels' often misses the mark
Not every pelvic floor needs squeezing. Some need relaxation and coordination first; others need strength, endurance, and pressure control. To make choices easier, we’ve compared three common paths below—the wait-and-see route, DIY Kegels-only, and guided pelvic health physiotherapy. Personalization matters.
- Approach What it involves Pros Risks/Limitations Typical timeline
- Wait-and-see Minimal change; hoping symptoms settle naturally No immediate cost or time commitment Symptoms can persist or worsen; activity avoidance grows Months to years; unpredictable
- DIY Kegels-only Generic squeezing practice without assessment Simple, accessible, can build awareness May worsen overactivity; ignores pressure, breathing, load Weeks to months; mixed results
- Pelvic health physiotherapy Assessment, education, and a tailored plan Addresses root causes; guided, progressive program Requires visits, home practice, and consistency 6–12+ weeks with clear milestones
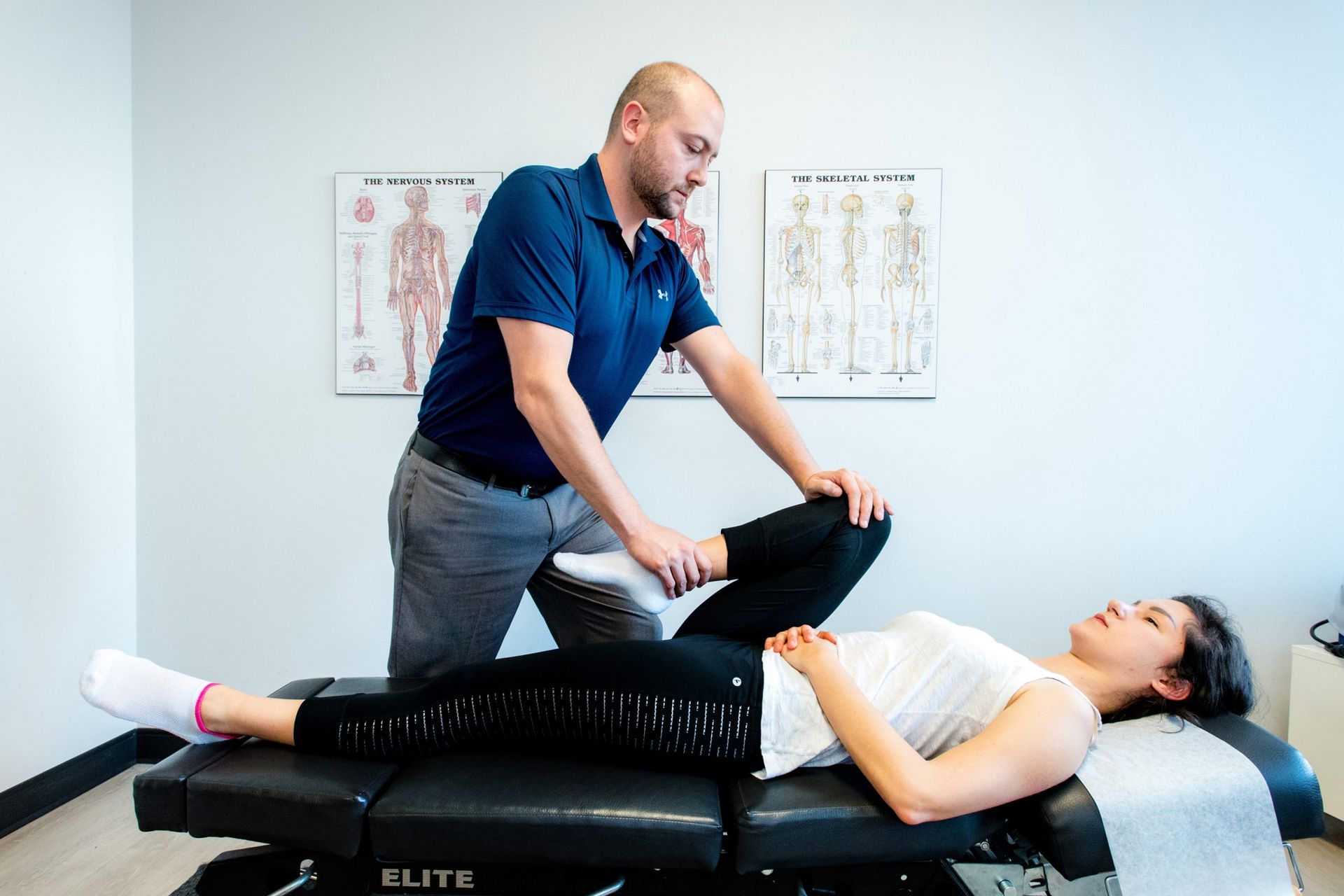
What to expect in pelvic physio—consent, clarity, real progress
So what actually happens in those 6–12 weeks? First, we sit down and listen—your birth history, current symptoms, fears, and goals (leak-free runs, painless sex, lifting your toddler). Then we do a movement and posture screen: how you breathe, squat, roll, and cough. We check pressure strategies (do you breath‑hold?), and we assess your hips, abdomen, and low back with gentle, external tests. If it fits your plan, we’ll discuss an internal pelvic floor exam (a gloved, one‑finger assessment) to check coordination and tone. It’s always your choice. If you prefer no internal exam, we use external options and still build a precise plan.
During the first visit, we’ll also map your starting point with simple measures: leak‑free cough test, diastasis depth (abdominal gap), single‑leg balance, and hop tolerance if appropriate. Wear comfortable clothes; you won’t need to change unless you want to. Prefer virtual? We can complete history, posture, breathing, and most movement screens on video, then tailor your home program. If at any point something doesn’t feel right, we pause, adapt, or stop—no questions asked. Consent is an ongoing conversation, not a one‑time form. You’ll leave visit one with 2–4 targeted exercises, pain‑easing strategies for this week, and a clear plan for the next session.
🛡️ Safety First
You’re in control—always. Internal assessment is optional and never required. We can make strong progress with external techniques, breath work, biofeedback cues, and graded exercise, then revisit options when you’re ready—or keep it external the whole time.
Treatment blends five pillars. First, downtraining when muscles are overactive: 360° breathing, pelvic drops, hip and rib mobility to reduce guarding. Second, progressive strength and coordination: glutes, core, and pelvic floor endurance with clear reps, sets, and tempos. Third, pressure management: exhale on effort, posture tweaks, and pacing to stop breath‑holding. Fourth, smart toileting: footstool, stool‑softening strategies, urge delay drills, and bowel mechanics. Fifth, return‑to‑movement planning: graded walking, lifting, and impact so you hit milestones like leak‑free stairs and 20 calf raises per side. We typically start weekly or bi‑weekly, then space visits as symptoms settle.
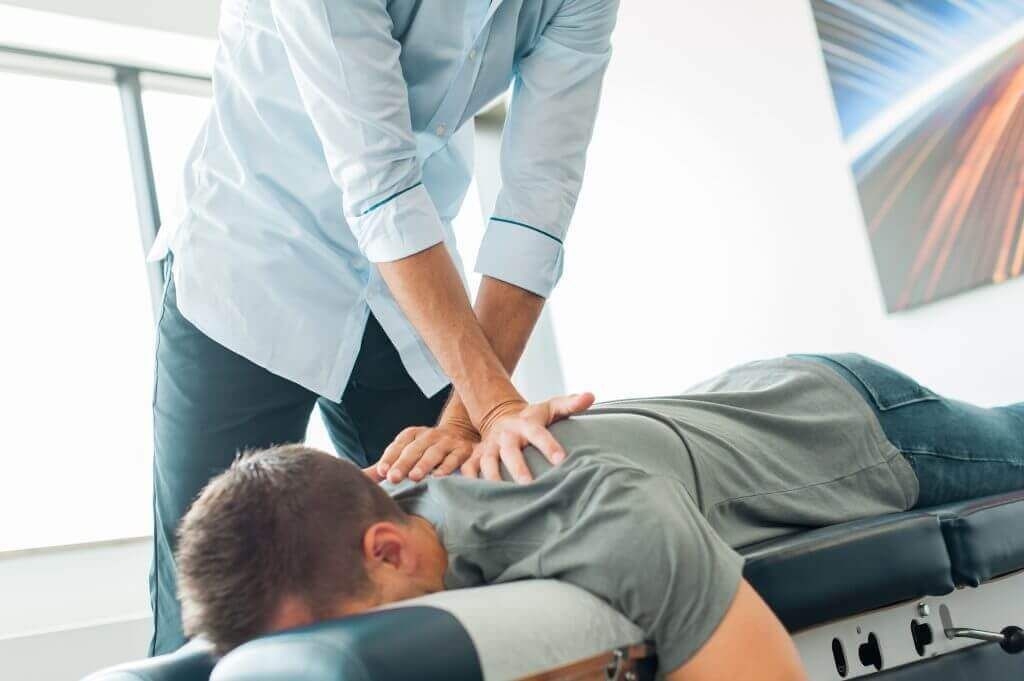
When hands-on care can help, we treat the tissues that share the load—pelvic floor, hips, abdomen, and low back—with gentle, targeted techniques to reduce pain and improve mobility. To see how we do it, visit our manual therapy Toronto
page. We pair manual work with breathing and strength so changes stick—walking with a stroller, lifting a car seat, or returning to sport.
Your trimester-by-trimester pelvic floor game plan
You’re breathing better and building strength—now let’s make it stick through each trimester while you’re walking with a stroller or lifting a car seat. We’ll target four pillars: coordination and breath, pressure management, pelvic girdle support, and sleep/positioning. Example: week one might be 2–3 minutes of 360 breathing, a footstool for bowel comfort, and 5–10 minute walks as tolerated. Then we layer strength and supports as your body changes.
- Trimester 1: Gentle coordination, nausea-aware strategies, walking as tolerated
- Trimester 2: Core-and-floor synergy, pelvic girdle support, progressive strength
- Trimester 3: Relaxation techniques, perineal prep, labour/birth positions and breath
- Prefer a step-by-step plan with coaching and accountability? Explore our pregnancy rehab downtown Toronto pathway—clear milestones, same-day options, and virtual visits when you need them.
Your first year after birth: a clear, compassionate roadmap
You wanted a step-by-step plan in pregnancy—let’s carry that clarity into postpartum. Every recovery looks different (vaginal or Cesarean birth, sleep, feeding, stitches), so we pace by symptoms, not pressure. We use checkpoints—rest, coordination, strength, impact readiness, and sport—to guide safe progress. Here’s the typical 0–12+ month flow we customize for you. If red flags appear—heavy bleeding, fever, worsening calf swelling, severe headache—contact your OB (obstetrician) or midwife and urgent care. We’ll be your steady guide.
- 0–6 weeks: Rest, breath, circulation, gentle mobility; C-section/perineal care
- 6–12 weeks: Coordination, graded walking, early strength; scar and tension work
- 3–6 months: Load progression, impact-readiness screens, sexual health check-ins
- 6–12+ months: Performance goals, sport return, symptom-free living
If pain lingers—deep pelvic ache, sharp C-section or perineal scar sensitivity, or painful sex—don’t wait it out. We offer compassionate, consent-led care; start with pelvic pain treatment Toronto
to see proven options. Relief is possible. When symptoms are calm, we’ll guide your return to running.
Ready to run? Your criteria and step-by-step plan
Symptoms are calm—so what’s the green light to run? Impact asks your pelvic floor, core, hips, and trunk to share load smoothly. Start with this 5-minute home screen; if you pass now, begin run-walk intervals, and if not, we’ll coach the gaps.
- Walk 30 minutes briskly without symptoms
- Cough/jump in place 10 times leak-free, pain-free
- Single-leg stand 30 seconds each, stable
- Sit-to-stand x10 without coning or heaviness
- Hip bridge x10 with breath control maintained
- No vaginal/abdominal heaviness the day after activity
It’s all connected: pelvis, hips, back, sciatic nerve
If your day‑after check brings back heaviness, hip ache, or low‑back twinges, the issue isn’t just the pelvic floor. Pregnancy posture and pelvic girdle mechanics—tilted pelvis, tight hips, breath‑holding—can crowd the sciatic nerve, sending pain or zings down one leg. We pair pelvic physio with hip and trunk work, and when needed, coordinated sciatica treatment Toronto,
so walking with a stroller or desk days feel easier. Next, simple drills you can start.
Your home program: simple steps that work
You asked for simple drills—here they are. These are safe starting points; the exact reps, holds, and progressions work best when tailored by a pelvic health physio. Begin small: 2–3 minutes of breath work and a 10‑minute walk today. If symptoms flare (leaking, heaviness, pain), scale back 20–30% and message us. We’ll personalize volume, tempo, and when to add impact.
- 360° breathing practice (2–3 minutes, 2–3x/day)
- Toileting posture and urge-suppression strategies
- Daily walking with posture and arm swing
- Hip abductor and extensor strength (e.g., clamshells, bridges)
- Gentle mobility for thorax and hips
- Pressure management in daily lifts/carries
- Sleep and feeding ergonomics to reduce neck/shoulder strain
Want coaching, progressions, and accountability? Explore our therapeutic exercise program—built for pregnancy and postpartum—at therapeutic exercise downtown Toronto. We’ll set reps, tempos, and weekly goals, then adjust based on your 48‑hour symptom check.
Physio and prenatal chiro: pain relief, alignment, load transfer
If your 48‑hour symptom check still flags pelvic heaviness, pubic bone pain, or rib tightness, that’s our cue to add prenatal chiropractic. Gentle mobilization (graded joint glides) and, when appropriate, manipulation (a quick, precise joint movement) free the SI joint (sacroiliac, where spine meets pelvis), ribs, and thoracic spine (mid‑back). We pair that with soft‑tissue release for glutes and pelvic floor neighbors. Result: your physio drills land—exhale to lift the car seat without pinching, 20‑minute walks without zings, fuller 360° breaths to reduce pressure.
Want a coordinated plan? We’ll align your exercises with targeted hands‑on care from our prenatal chiropractor downtown Toronto—shared notes, same goals, clear timelines. You’ll know exactly when to book each visit and what to practice between.
Real results: quick composite case snapshots
When you know exactly when to book and what to practice, change happens fast. These mini-stories are composites that reflect common paths we see in downtown Toronto. Timelines vary with symptoms, delivery type, sleep, and life demands. We’ll match the pace to your body and your goals.
- Runner, Trimester 2, pubic symphysis pain: loading plan, pelvic belt, breath strategies, sleep tweaks; symptom-free daily walks by week 4, impact testing and light jog intervals by week 8.
- Postpartum at 12 weeks, leaking with sneezes: downtraining, coordination, pressure control, gradual HIIT; leak-free daily life by week 10 of care, graded jumps and shuttle runs by week 12.
- C-section scar tightness with low-back ache: scar mobilization, trunk mobility, glute strength; sleeping without ache by week 6, stroller walks 20 minutes by week 4.
Curious what your path might look like? Explore our physiotherapy options here: physiotherapy Toronto.
We map a plan around your symptoms, schedule, and goals—same-day spots and virtual visits available. Still wondering about safety, costs, or bringing your baby? We tackle those FAQs next.
Your pregnancy and postpartum pelvic health FAQs, answered
- You asked about safety, costs, and bringing your baby—great questions. These answers are general; your body and birth story are unique. We’ll personalize everything in a 60‑minute pelvic health assessment or quick phone consult, and you’ll leave with clear next steps.
- Yes—when indicated and with consent. We screen, avoid red flags, and can treat externally only in pregnancy or postpartum if you prefer. Your comfort and goals set the plan.
- No—Ontario allows direct access to physiotherapy. Many plans accept direct billing; if your insurer needs a referral, we’ll tell you exactly what to request.
- Most start at 4–8 weeks postpartum. Start sooner if you have pain, leaking, constipation, heaviness, or scar concerns; we also offer virtual check‑ins in the first two weeks.
- Sometimes. If muscles are tight or overactive, squeezing more can worsen symptoms. We focus on coordination—relax, then engage with breath—and avoid Kegels when pain or heaviness increases.
- Diastasis (abdominal gap) is common. Our goals are tension you can generate, symptom‑free function, and load tolerance. We test tasks, not just measure width, and progress strength with breath.
- Support baby with pillows, bring them to you, keep wrists neutral, and change sides. If symptoms persist, see our neck pain treatment Toronto options for targeted relief.
Symptoms persisting? Your next step starts today
If those FAQs—and the neck-friendly tips—still leave you wondering, we’ll make it simple. Book a 60‑minute pelvic health assessment for a personalized plan, clear milestones, and symptom‑based pacing. Same‑day spots may be available, and we offer direct billing with most insurers—no referral needed. Inclusive care for every birth story (vaginal or C‑section), every stage (pregnancy to one year postpartum and beyond), and every body.
Prefer to talk? Call 416-975-0499 and we’ll book you fast. Outside Toronto or early postpartum? We offer secure virtual rehabilitation so you can start from home.
Prefer to talk? Here’s the evidence we rely on
Before you book or start a program at home, you might want to see the evidence we use. We’ll add links to current guidelines and consensus papers on this page. For example, the 2019 postnatal return-to-running consensus sets criteria-based readiness.
- Canadian guidelines on postpartum care and incontinence (e.g., SOGC)
- Physiotherapy practice resources on pelvic health (e.g., CPA divisions)
- Postnatal return-to-running consensus statements
- Peer-reviewed research on pelvic floor training and outcomes
- Public health resources on perinatal physical activity