Why Physiotherapy Works for Chronic Pain: Relief That Lasts
John Velasquez • March 2, 2026
Your alarm isn’t broken—it’s just turned up too loud
One in five Canadian adults live with chronic pain (Canadian Pain Task Force). This might sound familiar: you wake stiff, commute, sit through Zooms, and by 3 pm your neck or back is burning—then the evening chores finish you off. You’ve tried rest, pills, even gadgets, but relief never sticks. We see you. At Rosedale Wellness Centre in downtown Toronto, we help you calm an overprotective alarm system and rebuild capacity, step by step. Ready for a practical plan?
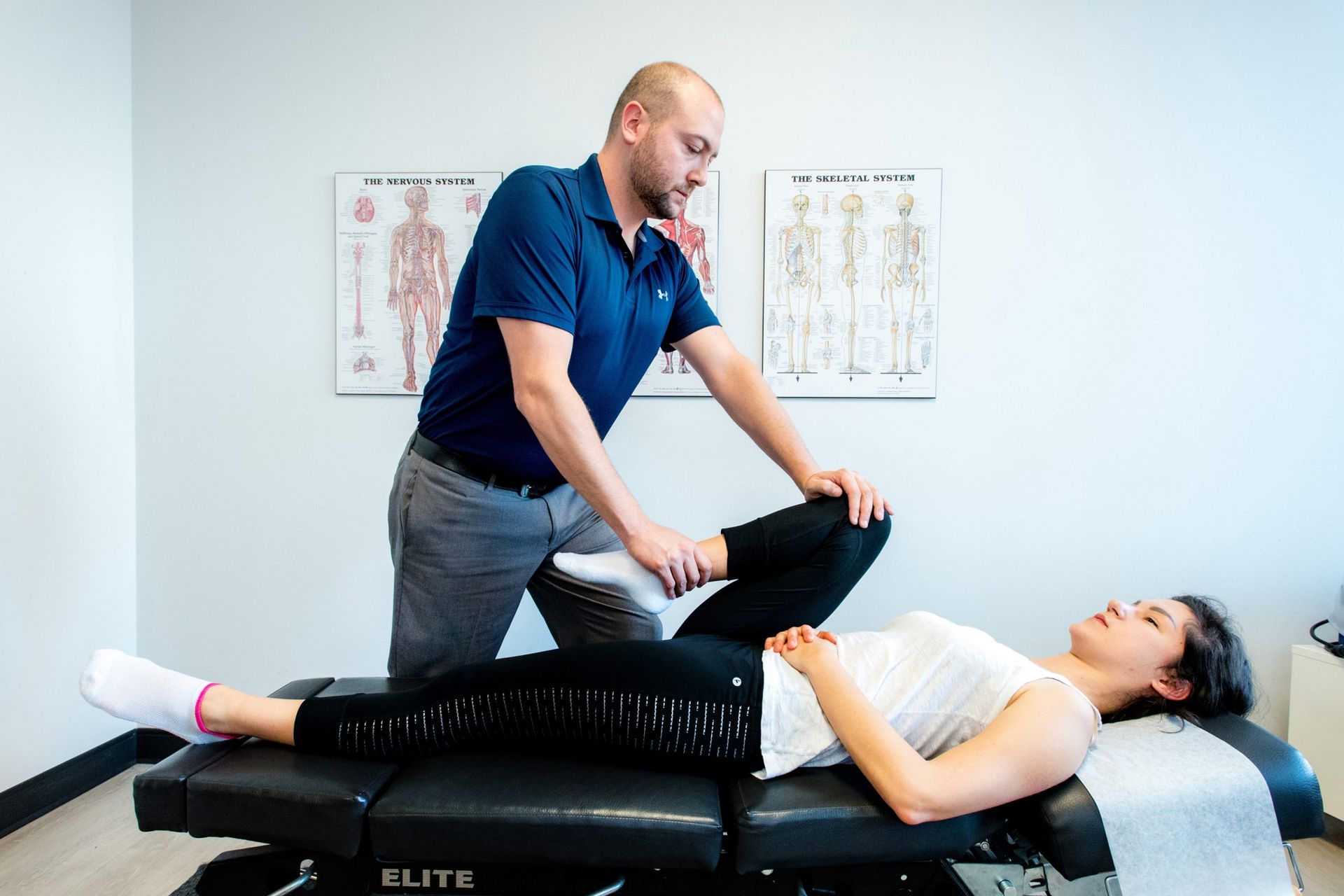
Physiotherapist guiding a patient through gentle movement for chronic pain relief
We’re moving past passive, medication-first care toward active, non‑pharmacologic treatment (movement, education, and smart loading). Physiotherapy works by retraining sensitivity and building strength with graded exposure—small, safe wins that add up in 6–12 weeks. We’ll show you exactly how: simple weekly steps, what good soreness feels like, and when to expect turning points. Same-day assessments, direct billing, and virtual visits make it doable from downtown or home. First question we’ll answer: why does chronic pain persist even after tissues heal?
💡 Key Takeaway
Physio treats root causes by calming sensitivity and rebuilding capacity. Expect a clear 6–12 week roadmap with pain education, graded loading, and short-term relief tools. Next step: book a same-day assessment or a free 10‑minute phone consult.
What chronic pain is and why it matters now
Before you book anything, let’s ground this: chronic pain means pain that sticks around for more than three months. By then, your alarm system (your nervous system) can turn the volume up—even when tissues have mostly healed. It’s not just bones and muscles. Pain is biopsychosocial—what your tissues can handle (load), plus sleep, stress, mood, and beliefs about movement. Long Zoom days, hybrid commutes, and skipped workouts in Toronto life all feed it. The good news: sensitivity can be retrained and capacity rebuilt.
Why it matters: it steals days from work, workouts, and family plans. You cancel rec league nights, leave early, and book more appointments. In Canada, chronic pain drives high healthcare use and disability claims. But the personal cost—confidence and connection—hurts most.
Most people then chase short-term symptom control—rest, pills, heat—without restoring capacity or confidence. That gap keeps the alarm loud and the body underprepared. So what actually keeps pain looping, even when scans look fine? Let’s break that down next.
Why does pain persist even after scans, pills, or rest?
First, central sensitization means your alarm is too sensitive; a light stretch reaching for a mug can sting like danger. Second, deconditioning lowers tissue capacity; after weeks avoiding stairs, two flights feel like a mountain. Third, guarded movement keeps muscles braced; you clench your back to pick up laundry, so everything feels tighter. Finally, fear-avoidance grows; you skip a short walk because “what if it flares,” which shrinks your world. Together, your body is trying to protect you, but the strategy backfires—more sensitivity, less capacity, more worry. That loop is fixable with graded exposure and strength.
And the tough part? Sensible choices in the moment can quietly backfire when repeated for months.
- Over-Resting: Prolonged rest lowers tissue capacity and increases stiffness, so smaller tasks feel harder.
- Chasing Scans: Imaging often shows age-typical changes that don’t equal pain or dictate recovery.
- Passive-Only Care: Relief without loading builds no capacity, so pain returns with normal life.
- Medication-First: Helpful short-term, but side effects and limited function gains keep you dependent.
- Catastrophizing Beliefs: Expecting damage from normal movement fuels fear, sensitivity, and disability.
Feeling stuck after doing “everything right”? You’re not the problem—the plan is. It takes a coordinated, graded approach that rebuilds capacity while calming sensitivity. That’s where our physio-led, team-based care breaks the loop and moves you forward.
Why quick fixes fade and real change sticks
If the plan is the problem, why did rest, pills, or a cortisone shot help only briefly? Medications and injections can settle a severe flare; surgery is essential for some structural issues. But for most long-standing back, neck, or joint pain, lasting change comes from active rehab—graded movement, education, and strength. We use these tools alongside short-term relief, not instead of them, so you can move more with less fear.
Now, how does this turn into less pain and more life? Next, we’ll unpack the physiotherapy mechanics—graded exposure, strength, pain education, and short-term relief tools—so you see the step-by-step path to lasting change in 6–12 weeks.
How Physiotherapy Re-Trains Pain
To turn less pain and more life into reality, we start with graded exposure—gradually reintroducing movements you’ve avoided, like 5‑minute walks that become 7, then 10. Next, we build load tolerance by progressively strengthening tissues—think two sets of 8–12 sit‑to‑stands or calf raises—so they handle daily demands without flaring. We refine motor control—how you coordinate hips, spine, and shoulders—so better movement patterns offload sore areas when you lift groceries, reach overhead, or sit long hours. Finally, threat education—clear explanations, a flare plan, and the 3/10 pain rule—reduces fear, keeps you engaged, and rewires how your nervous system interprets signals.
- Desensitization: Safe, repeated movement lowers your nervous-system alarm.
- Capacity-Building: Progressive loading strengthens tissues and reduces flare risk.
- Coordination: Better patterns shift load away from irritated joints and tendons.
- Education: Clear rules and context reduce fear and improve follow-through.
Want guidance tailored to your job, commute, and schedule? Our physiotherapy Toronto
team blends relief and strength, with same-day bookings and direct billing, so you can start now and see change within 6–12 weeks.
📚Evidence Snapshot
Lancet series and NICE guidance prioritize active, non‑pharmacologic care—education, exercise, and limited imaging—because movement-based programs outperform passive-only care for persistent back, neck, and joint pain.
The Four Pillars of Lasting Relief
So how do we turn that evidence—education, exercise, and limited imaging—into a plan you can follow? We blend four pillars, adjusting for your goals, pain irritability, and Toronto life. Think 10–20 minute home sessions, strategic clinic visits, and clear milestones that build confidence week by week.
- Pillar 1: Manual Therapy: Gentle joint and soft‑tissue work reduces guarding so you can move. Our manual therapy Toronto sessions prime you for exercise.
- Pillar 2: Therapeutic Exercise: Graded strength and mobility build capacity. We tailor sets and progression with therapeutic exercise downtown Toronto to match symptoms and goals.
- Pillar 3: Education & Self-Management: Pain science, sleep and stress support, pacing with the 3/10 rule, and a flare plan so setbacks don’t derail progress.
- Pillar 4: Adjunct Modalities: Acupuncture, laser, and targeted massage decrease irritability short‑term to enable exercise. Useful helpers during flares—never substitutes for loading and movement.
✅ Safety & Personalization
Your plan matches your current tolerance: we adjust reps, tempo, and visit frequency to pain levels and energy. We track strength, function, and symptoms together, so you see steady wins and know when to push or pause.
From Assessment to Momentum
Because we adjust reps, tempo, and visits to your tolerance and track your wins, here’s how the first 6–12 weeks usually unfold. In visit one we map goals (carry groceries, sit 60 minutes) and capture baselines: pain 0–10 and PSFS (Patient‑Specific Functional Scale—your chosen tasks). Early on it’s 1–2 visits a week and 10–20 minute home sessions. We right‑size to irritability: stiff backs start with breath and short walks; runners begin light loading. Expect calmer flares by weeks 2–3 and measurable function by weeks 4–6. Next, condition‑specific timelines.
Step 1: Assessment & Goal-Setting: Define 2–3 life goals, capture baselines, agree on schedule and flare rules.
Step 2: Early Desensitization: Gentle mobility, diaphragmatic breathing, heat/ice as needed; 3/10 pain rule and 24-hour check.
Step 3: Capacity Building: Add sets or weight weekly; track next‑day soreness and function; adjust volume if pain lingers past 48 hours.
Step 4: Skill & Confidence: Motor control, balance, and pacing; reintroduce stairs, lifting, or runs with clear progressions and milestones.
Step 5: Sustain & Prevent: Taper visits, set weekly strength and walk targets; know when to scale up or down during flares.
🗓️Access Made Easy
Same-day assessments when available, direct billing to major insurers, and flexible in-person or virtual rehab. Early and late appointments mean you can start this week and stay consistent—even during travel or busy stretches.
How long will this take?
Since scheduling is covered with early/late hours and virtual, the next question is timing—how long will change take? It varies by history, irritability, sleep, and consistency. Use these patterns as planning guardrails and a starting point for your plan. Example: desk‑related back pain often sleeps better by weeks 2–3; by weeks 4–6, 30–45 minute sits feel easier. We’ll personalize these numbers together.
- Condition Typical program length Visit frequency Home exercise (min/week) Expected milestones
- Chronic low back pain 8–12 weeks 1–2×/week early, taper later 90–150 min/week across 5–6 days Weeks 2–3 better sleep; 4–6 stamina; 8–12 hobbies
- Knee osteoarthritis 12+ weeks 1×/week, occasional booster blocks 120–180 min/week strength and walking Weeks 3–4 stiffness down; 6–8 strength; 10–12 longer walks
- Post‑surgical (e.g., rotator cuff) 12–24+ weeks per protocol Protocol-based (surgeon and physio) 120–180 min/week, phase‑specific Protected range, then strength; milestones by protocol
- Sciatica/radiculopathy 6–12 weeks 1–2×/week early, taper 90–150 min/week mobility and loading Weeks 2–3 centralization; 4–8 sitting/walking tolerance
- Neck pain with headaches 6–10 weeks 1×/week, add as needed 60–120 min/week posture and strength Weeks 2–3 fewer headaches; 4–6 endurance; 8–10 resilience
Consistency wins: show up, do 10–20 minute home sessions, and track how you feel tomorrow. If life or symptoms spike, message us—we’ll adjust fast. Setbacks are normal; with small tweaks, your trend stays up.
Three real-world snapshots of progress
Consistency wins—and small tweaks keep the trend up. Here’s how that looked for three typical clients who followed a tailored plan. Your results will vary; these are patterns, not promises. Wondering if you’re a fit? Next, we’ll outline who benefits and safety flags.
- Case 1: Sciatica, desk worker: With graded extensions and walks, pain dropped 7/10→2/10 by week 8; sitting 60 minutes without zingers. Used short-term manual therapy and our sciatica treatment Toronto plan to stay on track.
- Case 2: Knee osteoarthritis, active grandparent: Strength plus pacing cut morning stiffness by week 4; walks grew 10→25 minutes by week 10. Massage for flares and our arthritis pain relief Toronto approach made consistency easy.
- Case 3: Neck pain with headaches, hybrid worker: Posture tweaks, flexor training, and acupuncture cut headaches 4/week→1 by week 6; NDI down 16 points. Our neck pain treatment Toronto plan fit office and home days.
Who benefits most from our plan
If those snapshots sounded like your office-and-home days, you’re likely a fit. Our physio-led plan adapts to age, activity, and history—including lingering pain after prior care. We scale load, add short-term relief when needed, and coordinate across our team. Beginners and older adults welcome; safety checks and medical referrals happen when appropriate.
- If you have low back or neck pain: Function-first rehab with posture, motor control, and sitting/standing tolerance.
- If you have arthritis: Joint-friendly strength, pacing, footwear/ergonomics, and flare plans for stairs, walking, chores.
- If you have sciatica/radicular pain: Centralize symptoms, then rebuild walking and sitting tolerance with graded loading.
- If you’re post-surgery: Protocol-based progressions, pain-calmed movement, and strength milestones coordinated with your surgeon.
- If you’re an athlete or weekend warrior: Return-to-sport plans with strength balance, workload tracking, and injury prevention.
- If you prefer natural, non-opioid care: Active strategies, education, acupuncture or laser to enable movement.
Can’t always make it in? Virtual rehab keeps coaching, exercise checks, and accountability on track. We blend in-person and video visits so travel, weather, or childcare never stall your momentum.
Safe, simple home wins to start today
To keep that momentum between in-person and virtual visits, we recommend these safe at-home starters. Personalize to your body, and if pain is new, severe, or unexplained, get screened first.
- Do: Use a 0–10 symptom dial to keep activity in mild-to-moderate range.
- Do: Spread movement snacks across the day, 2–5 minutes each, every 45–60 minutes.
- Do: Pair diaphragmatic breathing with gentle mobility to reduce guarding and tension.
- Do: Track 1–2 meaningful outcomes like sleep quality, morning stiffness, or walk time.
- Do: Progress one variable at a time—reps, load, or duration—then reassess next day.
To prevent setbacks when symptoms are irritable, pause these for now. We’ll reintroduce them once your baseline is steadier and your 0–10 dial stays calm the next day.
- Avoid: Sudden spikes in activity volume or intensity; increase no more than 10–15% weekly.
- Avoid: Long daily sitting without brief movement breaks every 45–60 minutes.
- Avoid: Holding your breath or bracing on every rep; exhale through the effort.
- Avoid: Catastrophic self-talk; swap for neutral facts like “sore, not broken—scaling 30% today.”
If you flare, scale back the last progression by 20–40%. Keep gentle movement (walking, mobility), add heat for stiffness or ice for hot, irritable pain 10–15 minutes. Resume progress when your 24‑hour baseline returns and sleep normalizes.
What the best evidence shows
After a flare settles and you resume progress, you might ask: does this approach actually work? The short answer: yes—high‑quality guidelines and reviews support active, multi‑component physiotherapy for chronic back, neck, and joint pain. Education plus structured exercise outperforms passive‑only care, delivering small‑to‑moderate improvements that add up in real life over 6–12 weeks. Adjuncts like manual therapy or acupuncture can reduce irritability short‑term so you can train. Consistency matters; people who complete regular home sessions and track goals see the biggest gains. We build our plans around this.
- Guidelines: Major bodies prioritize active, non-pharmacologic care first-line.
- Exercise Evidence: Meta-analyses show small-to-moderate benefits versus minimal or passive care.
- Education Synergy: Education reduces fear, improves adherence, and enhances exercise outcomes.
- Long-Term Benefit: Combined programs reduce recurrence, healthcare use, and time off work.
Want to see the receipts? Here are trusted sources to skim now. Bring questions to your assessment—and next, we’ll tackle common objections so you can act confidently.
- The Lancet Low Back Pain Series (2018): Global recommendations prioritizing active, person-centred care.
- NICE Guideline NG59 (National Institute for Health and Care Excellence): Low back pain and sciatica.
- Cochrane Review (2021): Exercise therapy for chronic non-specific low back pain.
- OARSI Guidelines (Osteoarthritis Research Society International, 2019): Non-surgical knee osteoarthritis management.
- JAMA Network Open (Journal of the American Medical Association, 2021): Exercise modalities for chronic back pain.
- Canadian Pain Task Force (2019–2021): National perspectives and recommendations on chronic pain.
Clear, candid answers to your questions
The sources are helpful; now you probably want simple, direct answers about pain, timelines, safety, and coverage. Here’s our quick version—so you can decide with confidence and book when you’re ready.
- Will it hurt?: Mild, short‑lived soreness is normal. We stay in a tolerable range using the 3/10 rule and adjust load, reps, or tempo fast if symptoms linger.
- How fast will I see change?: Small wins in 2–4 weeks—better sleep, easier sits. Lasting gains in 6–12+ weeks with consistent home work and progressive loading.
- Is it safe for arthritis or older adults?: Yes. We use joint‑friendly strength, balance, pacing, and rest days. Programs scale to your starting point and medical history.
- Do I need imaging first?: Not usually. We screen for red flags, measure function, and liaise with your physician or order imaging when findings would change the plan.
- Can virtual rehab work?: Yes—for coaching, exercise checks, and accountability between in‑person sessions. We blend video and clinic visits so travel, weather, or childcare never stall progress.
Get clarity with a same-day assessment
Since coverage is handled with direct billing, your next step is a personalized assessment. We’ll pinpoint drivers of your pain, set 2–3 life goals, and map a 6–12 week plan—available same day, downtown or virtual. If you want a preview, see our chronic pain treatment Toronto
approach. Prefer to talk first? Call 416-975-0499 for a quick chat.
Meet Rosedale Wellness Centre
Before you book your assessment, meet the team behind your plan. We’re Rosedale Wellness Centre—a multidisciplinary clinic for physiotherapy, chiropractic, acupuncture, massage, and laser—delivering natural, personalized care that fits your real life. We help people with back and neck pain, arthritis, sciatica, and sports strains rebuild capacity in 6–12 weeks with clear goals and graded exercise. Same-day appointments, direct billing, and our downtown home at 120 Bloor St E make getting started simple.