Benefits of Consistent Physiotherapy (and How to Make It Stick)
John Velasquez • March 2, 2026
What Really Happens When You Don’t Skip Physiotherapy
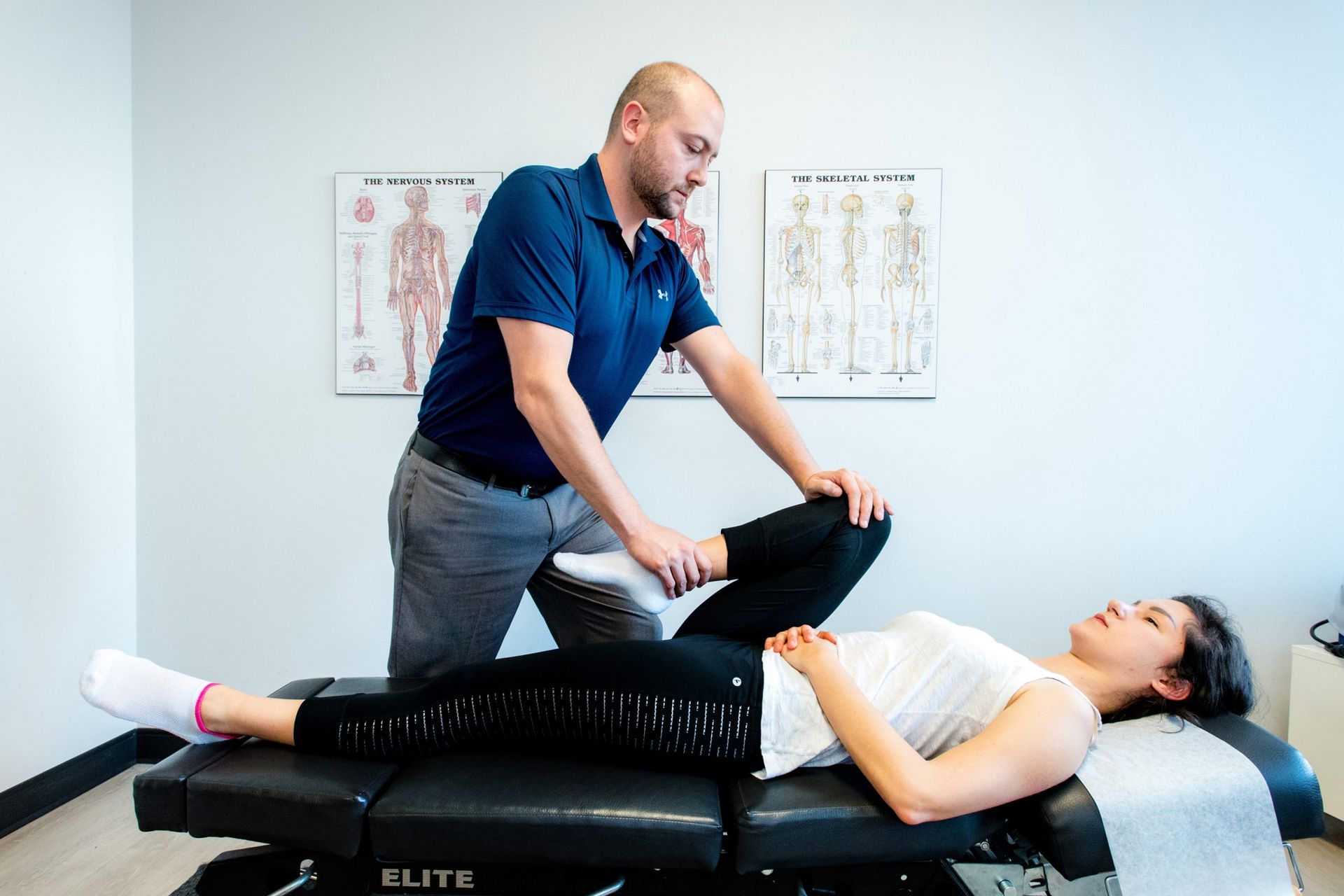
So what does “make it stick” look like day to day? We see it every week. Two people, same knee flare. Alex misses two weeks; long days at a desk, stairs sting, energy fades by 3 p.m. Sam st icks to 10-minute mornings and one weekly session. By week two, Sam climbs to the subway without wincing, posture steadier, stride smoother. That steady rhythm nudges strength, coordination, and confidence up—one small deposit at a time.
Sam’s week is simple: heel raises while coffee drips, eight-minute neck reset between Zoom calls, evening walk to the corner store. Nothing heroic. It adds up. By Friday, Sam reaches for a backpack with ease and moves first, thinks later. Alex guards every step, waiting for a perfect window. Different inputs, different nervous systems—one growing confidence, one rehearsing hesitation. Want that steady upward curve? You don’t need hours. You need a rhythm.
📈 By the numbers
Adherence—showing up and doing the plan—predicts better pain and function (Jack et al., 2010; Sluijs et al., 1993). Next, we’ll define what consistency means in physiotherapy terms and give you simple steps to hit it.
Consistency, Defined: More Than Just Showing Up
You just saw how adherence predicts results—so what does consistency actually mean in your week? It’s two parts working together: a steady clinic cadence (regular visits) plus home micro-doses (10–15 minutes most days). Those repeated, right-sized sessions teach your nervous system (your body’s control center) to move without guarding and give tissues (muscle, tendon, joints) enough load to adapt. Timing matters. Repetition builds self-management you can trust.
Practically, think 1 clinic visit per week for 4–6 weeks, then biweekly as symptoms settle, paired with a HEP (home exercise program) you can finish in 10–15 minutes. Anchor it to routines: calf raises while coffee brews, a two-minute posture reset every 60–90 minutes, and a 20-minute walk after work. That rhythm—small efforts, repeated—matches recovery cycles: load, then rest, then slightly more load.
At Rosedale Wellness Centre, our multidisciplinary team—physiotherapy, chiropractic, acupuncture, massage therapy, laser therapy, and virtual rehab—makes consistency doable. Same-day appointments prevent gaps, and direct billing removes admin delays. We coordinate the sequence so each service supports progressive loading, not distracts from it.
New to our approach? Start with our overview of physiotherapy Toronto
to see how clinic sessions and home plans work together.
The Hidden Cost of Inconsistency: Setbacks You Can’t See (Yet)
When you stop–start, skills fade and tissues stall. Motor learning (your brain–muscle coordination) decays without repetition, so movements feel clunky again. Tissues need progressive load (gradually increasing challenge) to remodel; long gaps lower their capacity. Stop–start patterns can also sensitize pain pathways—your alarm system gets jumpy. Example: an Achilles tendon aligns collagen with steady loading; skip a week, and tolerance drops, so the same stairs feel sharper.
Think of it like learning a language: daily 10-minute practice beats a once-a-week cram. Miss a few days and you don’t forget everything—you just feel slow, second-guess words, and tire faster. Your body works the same way. Inconsistency doesn’t just pause progress; it quietly rewinds it. That’s why flare-ups seem random. They’re not. Capacity dipped, life asked for more, and the system protested.
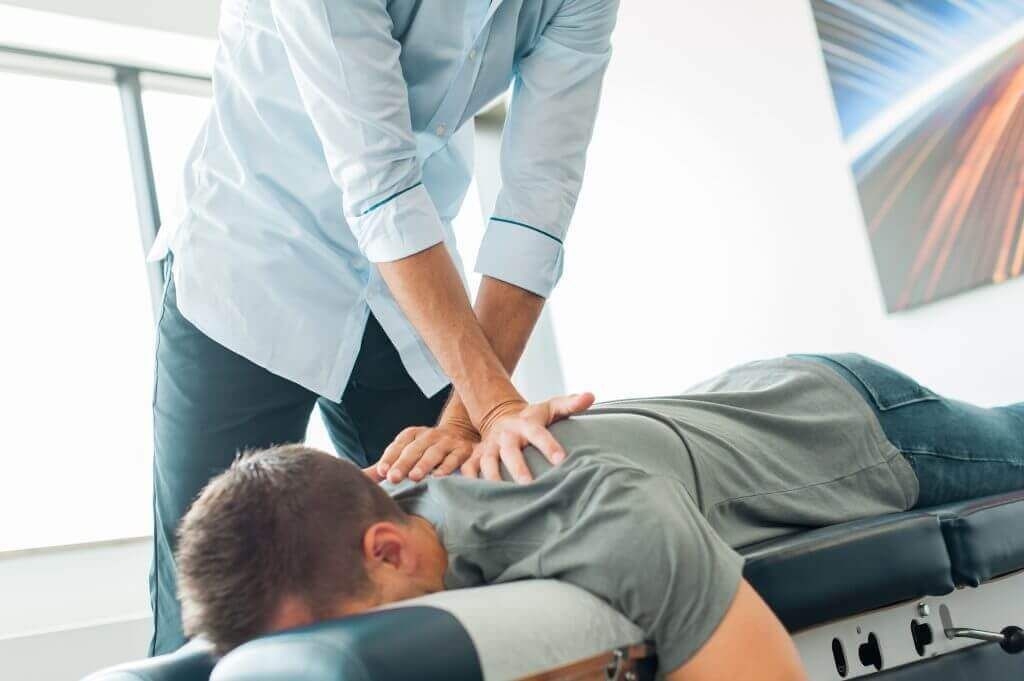
Picture a desk-heavy week. Your low back felt okay, then two missed weeks slide by. Saturday’s laundry, groceries, and vacuuming pile up, and by evening your back is hot and tight. It isn’t bad luck—endurance and control slipped, so routine chores suddenly overshot your capacity.
If back pain starts radiating down your leg, don’t wait. Read our guide to
sciatica treatment Toronto and learn how we calm nerves while rebuilding capacity.
- Deconditioning that makes daily tasks feel harder week by week
- Movement compensations that hide the problem but increase strain elsewhere
- Symptoms that become unpredictable, eroding confidence and routine
- Longer total recovery time (and higher overall cost) compared with steady care
Why “When I Have Time” Rehab Fails
Longer timelines and higher costs aren’t bad luck—they’re baked into “catch‑up” rehab. You can’t compress three missed weeks into one marathon session; tissues adapt to regular doses, not rare surges. The YouTube routine trap is similar: generic plans ignore your irritants, capacity, and stage, so dosing (how much), progression (what’s next), and feedback (what to change) go missing. Load management—how often, how hard, how long—needs a plan. Pain science backs graded exposure (gradually increasing challenge) over boom–bust spikes because steady exposure calms the alarm system while building capacity.
Picture this: you skip two weeks, then do 90 minutes of “make‑up” lunges, squats, and hills. Volume and intensity don’t match your current capacity, so your knee barks the next morning and walking the TTC stairs feels brutal. Now you’re guarding, not building. Contrast that with 15 minutes, five days a week: split squats at bodyweight, then light dumbbells, then tempo. Real‑time technique feedback—like keeping your knee tracking over toes and even weight through your foot—stops compensations before they snowball. That’s how you nudge adaptation without lighting a flare.
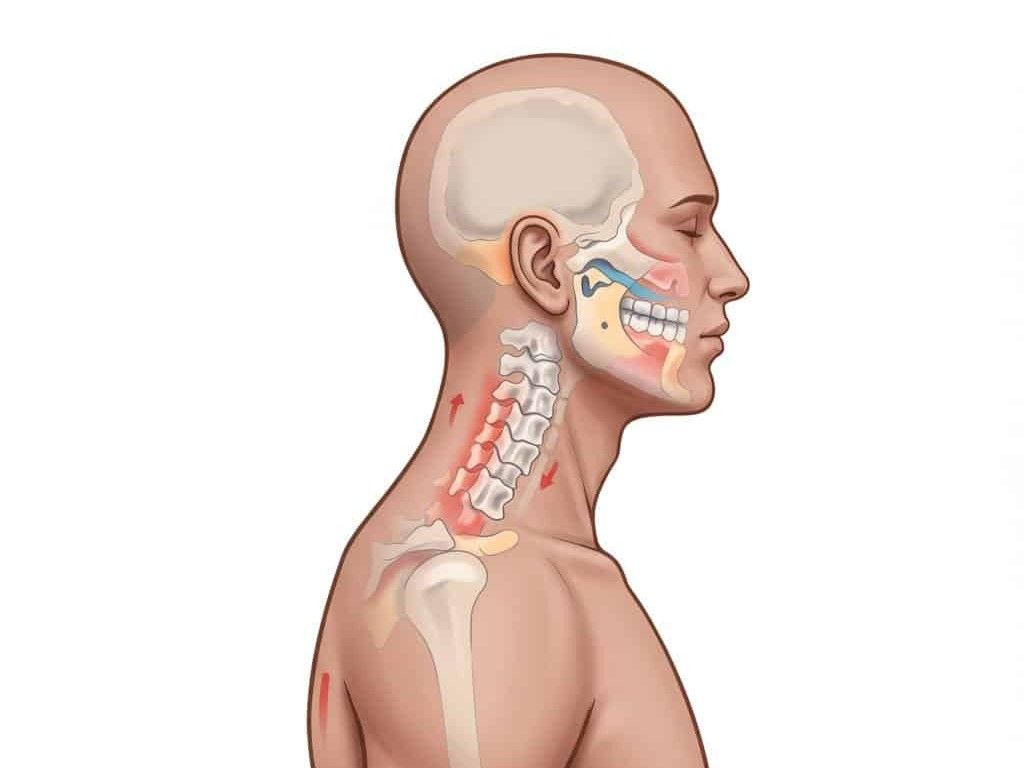
Office neck and shoulder strain is the classic boom–bust cycle: Monday–Thursday you grind, Friday you “fix it” with a hard session, then headaches return by Tuesday. We map steadier, lighter doses in our neck pain treatment
Toronto approach.
- You only exercise when pain spikes, not before it does
- Your program never progresses reps, range, or load
- You skip notes and technique feedback between sessions
- You need frequent days off work after DIY ‘mega’ workouts
- The Consistency Framework: 3 Pillars That Make Physio Stick
We replace ad‑hoc effort with three simple pillars: Appointment Cadence, Daily Micro‑Doses (a home exercise program you can finish in minutes), and Recovery Behaviours. Small, repeatable habits, tracked weekly, create the compounding effect your body trusts—and your calendar can keep.
Here’s how each pillar works in real life, with actions to take and simple measures to track progress.
- Pillar 1: Appointment Cadence — pre‑book 4–6 weeks, keep default time slots, and use same‑day or virtual swaps to protect streaks. Track attendance rate and gap length (days between visits).
- Pillar 2: Daily Micro‑Doses — 8–12 minutes, most days. Mix mobility, strength, and nerve‑friendly drills (gentle nerve glides = sliding nerves comfortably). Track streaks, reps, and loads.
- Pillar 3: Recovery Behaviours — prioritize sleep, stress downshifts, posture breaks, steps, and breathwork. Aim 7–9 hours, 6–8 posture resets, and 7–10K steps. Track sleep and step count.
Together, these pillars create a feedback loop: you log what you did and how it felt; we review, tune dosage and technique, and your symptoms get steadier. Fewer spikes. More capacity. Clear next steps.
Use this milestone map to set expectations, spot plateaus early, and know when to progress or pivot.
Phase Typical timeframe What improves What to watch Clinician check
- Weeks 0–2 Familiarity with exercises; initial pain relief Technique, swelling, sleep Post‑exercise soreness within 24–48 hours Confirm form; adjust dose
- Weeks 3–6 Noticeable function gains Strength, balance, confidence Overdoing on ‘good days’ Progress reps/load; refine goals
- Weeks 6–12 Return to most daily activities Endurance, range, pacing Complacency; skipped sessions Advance complexity; add prevention
- Months 3–6 Performance and resilience Sport/work tolerance Small relapses under stress Booster sessions; self‑management plan
- Months 6–12 Long‑term maintenance Lifestyle integration Gradual drift from habits Quarterly check‑ins; refresh program
🧪 Evidence note
Supported by NICE low back pain guidance and ACP guidelines: stay active, use exercise with graded exposure. Systematic reviews show adherence and progressive load drive outcomes across musculoskeletal rehab.
How Often Should You Go? It Depends on Your Condition
Those guidelines are clear about staying active with graded exposure. So how often should you actually come? Use this as a starting cadence; we’ll tailor frequency to your symptoms, goals, schedule, and benefits.
Condition Typical session frequency Home program dose Reassessment point Notes
- Acute ankle sprain (sport) 1–2 visits per week 8–12 minutes daily plus balance and calf work Reassess at 3–4 weeks Protect early; progress to strength, agility, and change‑of‑direction
- Low back pain and sciatica 1–2 visits per week 10–15 minutes daily core, mobility, and walking Reassess at 3–4 weeks Emphasize graded exposure and confidence with movement
- Post‑operative ACL or rotator cuff 2 visits weekly early, taper to 1 weekly Daily home protocol stages and precautions Reassess at 2–3 weeks Follow surgeon and physiotherapist criteria
- Desk‑related neck and shoulder pain 1 visit weekly plus virtual check‑in 8–10 minutes mobility plus ergonomic tweaks Reassess at 3 weeks Micro‑breaks every 60–90 minutes matter
- Chronic pain (persistent, 3+ months) 1 visit weekly plus education and pacing 6–10 minutes pacing, mobility, and gentle aerobic Reassess at 3–4 weeks Focus on function, not chasing pain to zero
- Pre‑surgical preparation (prehab) 1 visit per week 10–12 minutes strength, swelling control, and breathing Reassess at 2–3 weeks Build capacity and education before surgery
- If your goal is a safe return to sport, see our approach to sports injury treatment Toronto. Up next, we’ll turn these cadences into a simple weekly plan you can actually keep.
Build a Week That Works (Even When Life Gets Busy)
You asked for a simple weekly plan you can keep—let’s make it real. Anchor your plan to existing habits, batch 8–12‑minute micro‑sessions, and protect your clinic slot like a meeting. Our 3‑2‑1 Week works: three quick home sessions, two 20–30‑minute blocks, one visit. Miss a day? We’ll show you a 72‑hour restart next.
Use this quick checklist to turn good intentions into a rhythm that survives busy weeks.
- Stack your HEP (home exercise program) to a daily cue like coffee or commute.
- Stage bands and a kettlebell where you’ll use them—kitchen, desk, or doorway.
- Use a one‑tap phone timer and a simple paper checklist on the fridge.
- Book your next session before you leave; default to the same day and time.
- On rest days, review technique, breath, and posture—light reps keep the groove.
🤝Need a hand staying on track?
Same-day appointments and direct billing make momentum easier. Book online or call 416-975-0499, and we’ll map your 3–12 week rhythm around your schedule—plus virtual swaps when life gets crowded.
Fell Off the Plan? Here’s How to Restart (Without Overdoing It)
Life gets crowded—if you miss a week, use this calm, step‑by‑step 72‑hour restart to rebuild safely without guesswork.
Step 1: Reassess — book a same‑week check‑in (virtual or in‑clinic) to retest range, strength, and triggers. Compare to week‑one baselines, flag nerve signs (numbness, sharp leg pain), and we’ll set safe next steps.
Step 2: Reset the dose — cut HEP (home exercise program) volume to 50–60% for one week. Keep frequency, start with isometrics (tensing without movement), and use 8–10 minute sets on busy days.
Step 3: Rebuild cadence — pre‑book the next 2–3 sessions now. Protect the same day/time (e.g., Tue 7:30 a.m.), use same‑day or virtual swaps when needed, and let direct billing remove admin friction.
Step 4: Track the trend — log pain (0–10), function (sit‑to‑stand reps, step count), and sleep. We care about direction over days, not single spikes; consistent “same or better” beats random heroics.
Step 5: Prevent drift — set a 60‑second minimum on tough days: doorway pec stretch, 10 calf raises, 5 slow breaths. If you hit the minimum, you kept the streak. Momentum preserved.
Paused after surgery? Protocol restarts are normal—your surgeon’s criteria guide timing. Learn how our post-surgical rehabilitation Downtown
Toronto team resets milestones and safely rebuilds range, strength, and confidence.
What the Evidence Says About Consistency and Results
Those milestones we reset after surgery—or after any flare—exist because recovery follows patterns. You’ll often feel symptom change in 2–6 weeks, while functional strength and confidence typically build over 6–12 weeks. Pace varies with severity, other health conditions, stress, sleep, and job demands. What matters most? Showing up consistently and doing short, regular home work. That combo compounds.
Here’s a quick, at‑a‑glance table linking adherence to timelines and outcomes.
- Scenario Typical timeline With high adherence With low adherence Notes
- Acute soft‑tissue strain (e.g., mild muscle pull) 3–6 weeks to resume light activity Pain declines faster; function returns on schedule Pain lingers; progress up‑and‑down week to week Progressive loading (gradual increases) and rest cycles matter [1]
- Lumbar radiculopathy (sciatica‑type leg pain) 6–12+ weeks, depending on irritability Better function; fewer flare‑ups; steadier walking tolerance Recurring flares; fear of movement persists Graded exposure (stepwise challenge) and walking help [2]
- Post‑operative rehabilitation (e.g., anterior cruciate ligament (ACL), rotator cuff) Protocol‑dependent; phased milestones over months Milestones met closer to schedule; fewer setbacks Delays, stiffness, and confidence dips Early controlled movement per protocol (surgeon‑approved plan) [3]
- Neck pain from postural load (desk/commute) 3–8 weeks with posture and strength work Fewer headaches; better range and endurance Ongoing discomfort; frequent tension recurs Ergonomics (workspace setup) + micro‑breaks are key [4]
- Persistent pain (3+ months) with sensitivity 8–12+ weeks for measurable function gains Improved function and confidence despite pain level Activity avoidance; boom–bust cycles continue Education, pacing (planned activity doses), and graded activity help [5]
📚Sources to include
Please add five concise endnotes: JOSPT (Journal of Orthopaedic & Sports Physical Therapy) on adherence/loading; BMJ guidance; Cochrane reviews; NICE (UK guidance) low back pain; CPA (Canadian Physiotherapy Association) pacing/timelines. No inline links.
For Chronic Pain, Consistency Beats Intensity
Those guidelines and reviews we just cited are useful—and with persistent pain we measure success differently. Your nervous system can stay sensitized (the alarm rings louder and earlier) even after tissues heal. So we track wins by function, confidence, and participation: more stairs, longer walks, better sleep, steadier mood. What works isn’t a heroic push; it’s low‑dose regular activity plus graded exposure (stepwise challenges tied to symptoms). We pace, we breathe, we nudge capacity up, and we stop rewarding boom–bust cycles. When pain spikes, we adjust dose, not quit. Progress looks like more good days and fewer crash days.
Here’s the frame we use. Week one: 10‑minute walks daily, two 60‑second mobility sets, and one light strength block on alternate days. We cap increases at 10–15% weekly and follow the 24‑hour rule: if symptoms settle within a day, the dose was right. Flare plan? Keep frequency, cut volume to 70% for 3–5 days, add breathwork (4‑second inhale, 6‑second exhale), and protect sleep. Example: your back twinges after groceries; next day you still walk 10 minutes, switch to isometrics, and message us to reset loads. Confidence climbs. Flares shrink. Steady wins set you up for prehab and prevention.
Living with long‑standing symptoms? Book support now—our chronic pain treatment Toronto
team blends pacing, education, and movement you can sustain.
- Shrink the set: 60–90 seconds counts on tough days
- Switch focus: breathing and gentle mobility first
- Track function wins (stairs, sleep, walks), not only pain
Prehab and Prevention: Getting Ahead of Problems
If we’re tracking function wins—stairs, sleep, walks—not just pain, prehab and prevention are the next logical step. Prehab means 4–8 weeks of targeted strength, mobility, and cardio before surgery to speed recovery and protect the opposite side and nearby joints. We calm swelling, restore range, sharpen movement patterns, and build stamina so day-one rehab starts on stronger ground. Once your goals are met, we shift to maintenance: fewer visits, short home sessions, and quarterly check-ins to keep capacity ahead of life’s demands.
Example baselines: pain at rest and with movement, range of motion, single‑leg sit‑to‑stand reps, and a 6‑minute walk (how far you cover in six minutes). Your HEP (home exercise program) runs 3–5 days a week: two strength blocks, three 8–12‑minute mobility sessions, and daily 15–20‑minute walks. Prevention tune‑ups look similar: a monthly check focused on technique and load, plus seasonal blocks before ski or run season to build calves, hips, and balance.
Planning a procedure? Learn how our pre-surgical physiotherapy Toronto
program sets baselines, builds protective strength, and maps your day‑one rehab plan. Book a same‑day assessment and we’ll design your 4–8 week prehab around your schedule, with virtual options and direct billing.
How Consistency Looks in Real Life: 2 Short Examples
That “designed around your schedule” approach worked at a desk, too. A marketing manager with neck pain booked a same-day start, then did weekly physio x4, 10-minute home sessions, and micro-breaks every 60–90 minutes. By week three, headaches dropped from 7/10 to 2/10, screen time felt steadier, and she finished days without tension spikes. Result? Fewer headaches, better focus, and energy left for the commute.
Weekend runner, mild calf strain. We used the 3 pillars: appointment cadence (biweekly check-ins), daily micro-doses (calf isometrics, then raises), and recovery behaviors (sleep, steps). Graded return-to-run: walk-jog intervals, +10% weekly if symptoms settled within 24 hours. At week six, 5K pain-free, cadence consistent, confidence back. We shifted to monthly maintenance to protect mileage bumps.
🌟Why clients stick with it
Our physiotherapists coordinate with chiropractic, massage, acupuncture, and laser, and same-day or virtual swaps keep streaks alive. Direct billing and Bloor Street, TTC-friendly access remove friction so you can be consistent without rearranging life.
Quick Answers to Common Questions
With same-day and virtual swaps—and direct billing to cut admin—here are quick answers on timelines, frequency, equipment, and virtual care so you can book confidently.
- How soon will I feel better? Many notice relief in 2–3 weeks with steady home work and weekly visits; strength and endurance often improve by weeks 6–8. We set checkpoints at weeks 2 and 4 to adjust.
- How often should I come in? Most start 1x/week for 4–6 weeks; acute flares may be 1–2x early, post‑op (after surgery) 2x early then 1x. We taper biweekly as symptoms settle and match your benefits and schedule.
- Do I need special equipment? No. We start with bodyweight, bands, a towel, stairs, and a backpack for loading. If needed, we’ll suggest a $10–$30 band set—nothing bulky or expensive.
- Can I do virtual sessions? Yes—great for coaching, progressions, and accountability. We blend in‑clinic when hands‑on care helps. Traveling or slammed week? We can swap to virtual same‑day to protect momentum.
- What if my schedule is unpredictable? Pre‑book a default slot, then use same‑day openings or virtual swaps. We’re steps from TTC (Toronto Transit Commission) on Bloor Street, and direct billing saves time. Missed a week? Use our 72‑hour Restart.
Start Your Most Consistent Week Yet
Schedule unpredictable—or missed a week? Keep the streak—book a same‑day visit or virtual check‑in now. We handle direct billing, we’re steps from TTC, and we’ll map a personalized 3–12 week plan on day one. Prefer to call? Reach us at 416-975-0499. Ready to start feeling better—consistently?