TMJ Disorders: Expert Treatment & Exercises | Toronto Clinic
John Velasquez • March 28, 2026
TMJ Disorders: Causes, Symptoms, Treatment and Exercises
Your jaw symptoms are signals, not random annoyances
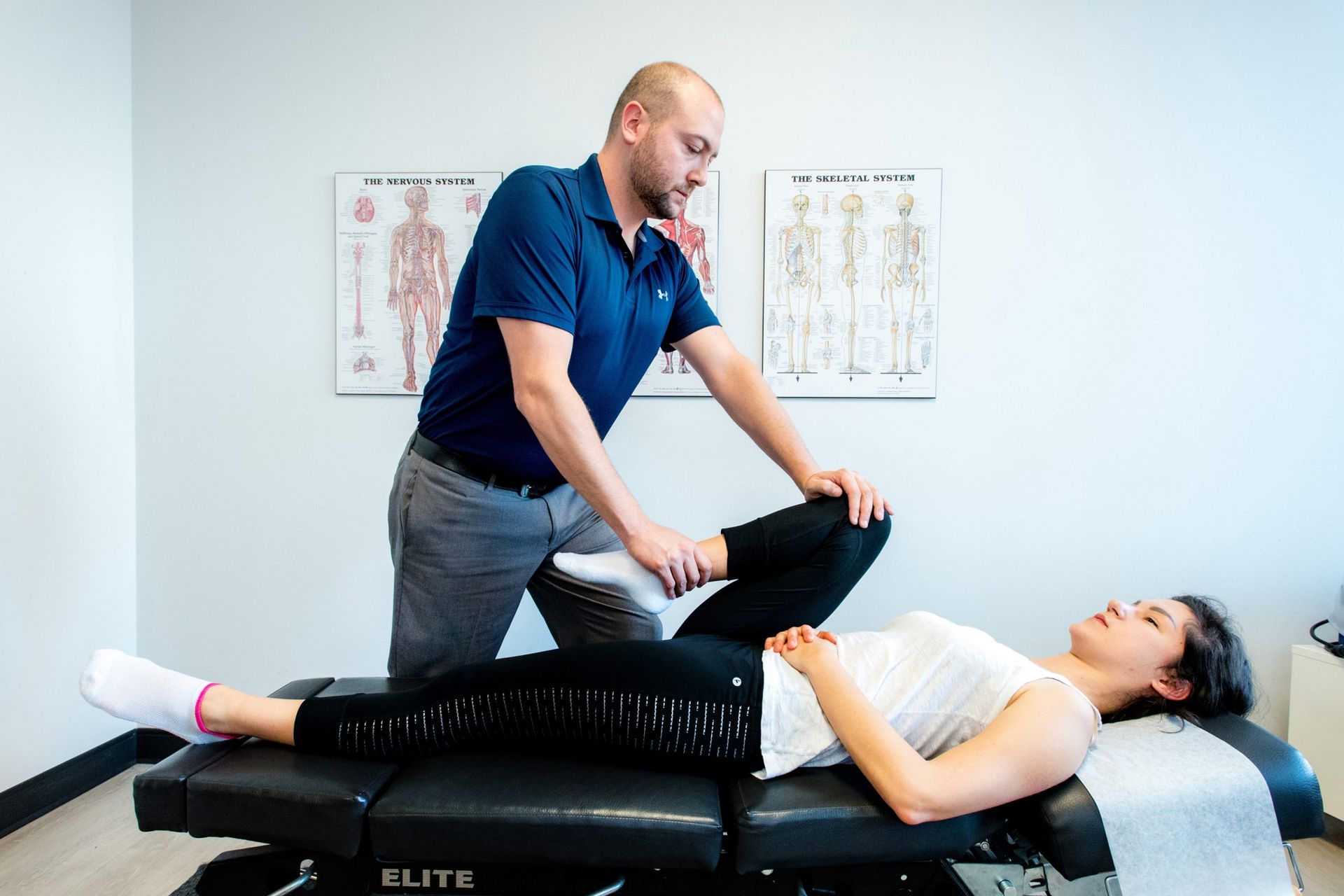
Does your jaw click on every Zoom call, then clamp shut when you yawn? Morning stiffness, temple tension, or a weird ear fullness that won’t quit? You’ve tried heat, soft foods, and those two-minute YouTube stretches. No luck. We see this every week in our downtown Toronto TMJ (temporomandibular joint) physiotherapy clinic. The jaw rarely acts alone—your neck, posture, and stress habits pile on. The good news: it’s treatable, naturally, and without relying on meds or surgery.
Those clicks and aches are signals, not defects. Often it’s TMD (temporomandibular disorder—jaw dysfunction), not just your TMJ (the jaw joint) misbehaving. Understanding the difference guides the fix. We connect the jaw–neck–head, coach habits, and use multidisciplinary, natural care so you can eat, talk, and sleep without thinking about it. We offer same-day assessments and direct billing right here on Bloor Street. Wondering what TMJ vs TMD actually means for you? We’ll make it simple next.
💡Good to know
About 5–12% of adults experience TMD symptoms—millions of Canadians, including many in Toronto.
TMJ vs TMD: the difference that guides care
You asked what TMJ vs TMD actually means—here’s the simple version we use in clinic. TMJ (temporomandibular joint) is the joint in front of your ear; TMD (temporomandibular disorder) is when that system is irritated. The joint is a sliding hinge with a small cartilage disc (a shock absorber) guided by muscles like the masseter, temporalis, and pterygoids (your jaw movers). Your neck coordinates the motion—if the neck is stiff or the head juts forward, the jaw works harder. Names matter because they point us to the right fix: joint, muscle, or both. If this all blurs together, you’re not alone. We translate it for you in plain English at your first visit.
Mechanics explain symptoms. A disc that slips forward and then snaps back is called ‘with reduction’—you hear a click, but movement stays normal. Irritated joint surfaces or a stuck disc can limit opening; overworked muscles can ache without any joint damage. Labels help us choose care: manual therapy to unload the joint, exercises for control, or calming tight muscles plus neck work. If you’re searching for TMJ physiotherapy in Toronto or jaw pain treatment downtown Toronto, our plan blends hands-on care with habit coaching and stress tools. Quick facts next, so you can spot your pattern.
Before we list symptoms and causes, here are quick facts that make the jaw–neck picture click.
- The TMJ is a sliding hinge guided by a small disc.
- Jaw position depends on neck and tongue posture.
- Stress and clenching load the joint more than chewing.
- Both muscles and joint surfaces can generate pain.
- Ear, head, and neck symptoms can share nerve pathways.
TMJ/TMD symptoms and when to worry
Symptoms vary depending on whether muscles, the joint, or both are irritated. Here’s what many people report.
- Clicking or popping when opening or closing.
- Pain or fatigue with chewing, talking, or singing.
- Limited opening under 35–40 mm or deviation off midline.
- Morning stiffness from clenching or grinding during sleep.
- Facial or temple pressure, aching in the cheeks.
- Ear fullness, ringing (tinnitus), or mild brief dizziness.
- Neck tightness with pain referring into teeth or jaw.
- Headaches that flare with jaw use or stress.
Some signs need urgent care; if you notice these, act.
- Trauma with inability to open or close the mouth.
- Progressive jaw locking that doesn’t resolve within 24–48 hours.
- Fever, spreading swelling, warmth, or suspected infection near the jaw.
- Unexplained weight loss, facial numbness, or severe persistent ear pain.
- New, severe headache with confusion, weakness, or vision changes.
🛟 Safety first
This page educates, not diagnoses. If symptoms are severe, changing quickly, or you’re unsure, see a qualified clinician or urgent care. We can help you decide the safest next step.
TMD is multifactorial, not one single cause
Most jaw pain comes from a mix of factors. Myofascial overuse (overworked muscles from clenching or chewing) creates tender, tight tissue. Disc displacement with reduction (the disc slides forward, then snaps back) often clicks but still allows full opening. Joint irritation or arthritis (the surfaces get inflamed or worn) can feel deep and achy. Bite changes or dental work can temporarily alter loading. Hypermobility (looser ligaments) makes control harder. Stress sensitizes the system, and poor nasal breathing keeps mouth muscles “on” all day. Often two or three of these travel together, which is why a single tool rarely fixes everything. We assess the blend in your case and match treatment accordingly.
Think about a typical week downtown. Eight hours at a laptop with a forward head, then a long dental appointment with your mouth held open. Add spring allergies that block your nose, so you mouth-breathe and keep the jaw slightly active. Or you start marathon rehearsals—violin, trumpet, or singing—and chew tougher foods between sets. Even athletes feel it after heavy lifts that drive tension into the neck and jaw. None of this is “bad,” it’s just load. When load outpaces recovery, TMD symptoms show up. The fix starts by reducing unnecessary load and improving control—especially through the neck and tongue. That sets up the jaw–neck–head work we’ll do together.
Start with what you can change today:
- Daytime clenching and night bruxism.
- Forward-head posture and poor ergonomics.
- Chewing on one side or hard, sticky foods.
- Mouth breathing and low tongue posture.
- High training loads for musicians, lifters, or contact sports.
- Insufficient recovery, hydration, and consistent sleep.
- Stress without daily relaxation or breathing routines.
The jaw–neck–head connection
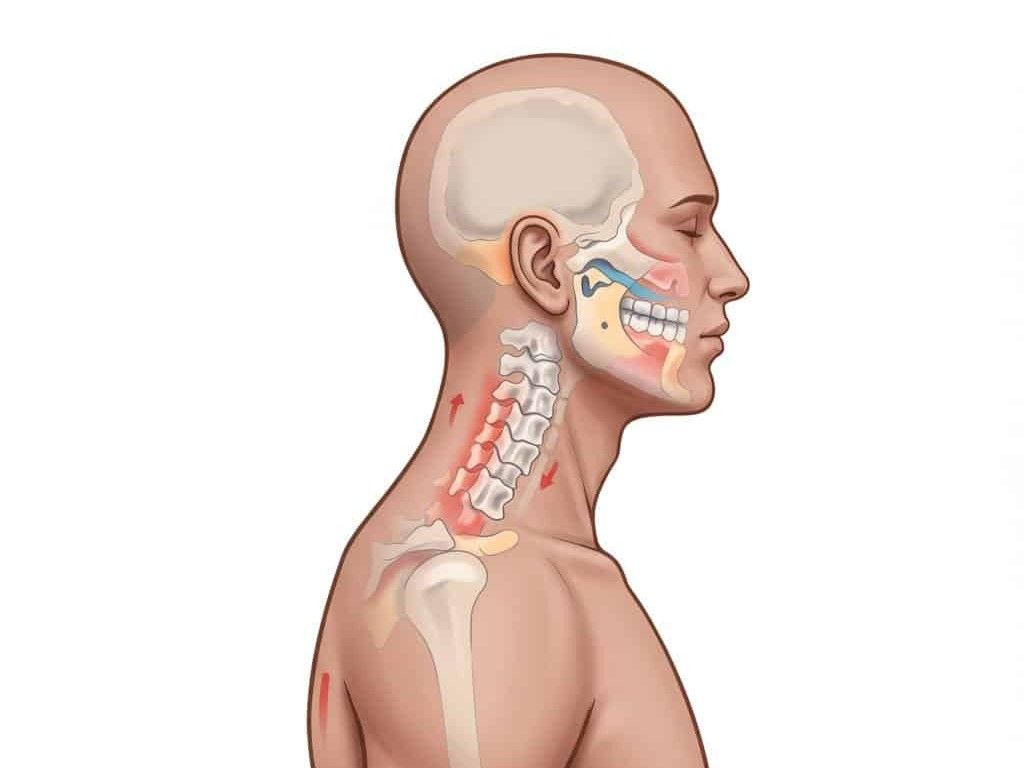
If stress keeps simmering without daily breathing resets, jaw muscles stay “on” and that tension often climbs into your head. Why does a tight jaw cause temple pain? The trigeminal nerve (the jaw/face nerve) shares pathways with upper neck nerves in a relay called the trigemino-cervical complex, so signals blend. That’s why clenching during emails can morph into a band-like headache or eye pressure. Try this: gently tap your molars together for 30 seconds; notice the temple heaviness that follows. When we unload the jaw with control and pacing, headaches usually ease. If you need more targeted support, our headaches and migraines treatment
layers jaw care with neck and lifestyle coaching.
Now, about your neck. A forward head posture (chin drifting ahead of your chest) forces the jaw to hinge in a compressed, off-axis way, increasing load on the joint and disc. Stiff upper cervical joints (the top two neck joints) and weak deep neck flexors (the small stabilizers) make control harder. Example: after an hour on a laptop, your mouth opens with a sideways drift and louder click; two minutes of chin tucks and scapular setting often quiets it. Breathing matters too—mouth breathing lowers the tongue, which destabilizes the jaw. Addressing the neck is not optional; it’s leverage. See how we blend this into care on our neck pain treatment
page.
Bottom line: your jaw, neck, and head share muscles, nerves, and habits—treating one in isolation stalls progress. We combine jaw control, neck mechanics, and breathing/stress work, with more detail on our headaches and migraines treatment and neck pain pages.
Avoidable habits that slow jaw healing
Since your jaw, neck, and habits work together, avoid these pitfalls while healing—then we’ll map your step-by-step plan.
- Skip gum and ice—constant chewing overloads the joint and fatigues the masseter (your main chewing muscle).
- Smaller bites, cut food; oversized bites force wide opening and can aggravate a sensitive disc and capsule.
- Ditch nail and pen biting—those tiny, frequent clench-releases keep pain circuits sensitized and strain front teeth.
- Avoid yanking your jaw to stop a click; aggressive stretching can inflame the joint and worsen disc irritation.
- Side or back sleep beats face-down; pressing your jaw into an arm compresses the joint for hours.
- Watch for clenching with earbuds or calls; rest tongue on palate, lips together, teeth apart.
- During flares, avoid jerky, bagels, taffy; choose softer proteins and alternate sides to share the load.
- Don’t ignore stress or mouth breathing; 4–6 paced breathing and nasal airflow calm overactive jaw muscles.
💡 Pro Tip
Support your jaw when yawning with a few fingers under the chin, and at rest remember: lips together, teeth apart, tongue gently on the palate.
Your step-by-step TMJ recovery plan
You’ve started practicing “lips together, teeth apart”—so what does a complete plan look like? We begin with a thorough assessment of jaw, neck, posture, and breathing, then teach you exactly how to lower daily load. Next, we calm pain with gentle manual therapy and simple, targeted exercises. Cervical rehab (neck mobility and deep neck control) restores alignment, while stress and breathing tools reduce clenching. When a splint or night guard could help, we coordinate with your dentist so rehab and dental care work together. Most people feel a change within 2–3 visits, then we progress. Same-day appointments and direct billing make getting started easy.
Care is integrated across our clinicians, so you’re not repeating your story. We pace it to your sensitivity: early visits weekly or biweekly, then taper as your home program takes over. You’ll get clear targets—opening in millimetres (mm), click loudness, chewing tolerance, and neck motion—so progress is visible. Prefer remote coaching? We support virtual rehab for teaching, tweaks, and accountability. Typical timelines: mild cases 2–4 weeks, moderate 6–12, chronic 3–6 months. You’ll always know why we’re doing each step and what comes next.
Here’s how the pieces fit—and why each one helps.
- Gentle, targeted hands-on care—see our manual therapy in Toronto—to calm irritation and restore glide.
- An individualized plan through physiotherapy in Toronto builds mobility, control, and strength at your pace.
- Habit coaching, nasal breathing, and sleep tweaks to cut daily jaw load.
- Graded chewing and talking tasks to build tolerance without flares.
- Acupuncture or low-level laser when needed to settle pain and inflammation.
- Collaborate with your dentist on splints or night guards when they help.
- Heat, safe self-massage, pacing strategies, and a simple flare plan.
- Follow-ups taper as you master self-care; brief check-ins keep momentum.
Want more detail? Explore our TMJ dysfunction treatment
for the full pathway.
Your first visit, step by step
You’ve seen the full pathway—now here’s exactly how your first visit runs. In about 45 minutes, we measure opening in millimetres, calm pain, and start your home plan today.
Step 1: Focused history—triggers, habits, stress, sleep, dental work; bring any splints or imaging.
Step 2: Measure jaw motion (mm), click/lock tests, deviation, and tongue posture.
Step 3: Gentle palpation—inside/outside mouth—to find tender muscles and joint sources.
Step 4: Cervical and scapular screen—posture, deep neck control, thoracic mobility links.
Step 5: Education + immediate relief—jaw support for yawns, heat/ice rules, 1–2 quick wins.
Step 6: Starter exercises—tongue-up opening, isometrics, chin tucks—with dosage and pacing.
Step 7: Milestones, timeline, follow-ups, and logistics—scheduling options, direct billing, taper points.
A safe, step-by-step jaw routine you can start
With your milestones and follow-ups mapped, let’s get you moving safely at home. Work only in a pain-free, smooth range and keep your opening on the midline—use a mirror for feedback. If you feel sharp pain, numbness, locking, or dizziness, stop and message us; a dull, easing stretch is fine. Slow wins here: think gentle, 3–4 second movements with relaxed shoulders. Example: if your jaw starts drifting left around 15 mm (about a fingertip), pause there and reset your tongue posture before the next rep.
Quality over intensity matters—small, perfect reps beat big, sloppy ones. Start with 1–2 sets daily and build to twice a day as symptoms settle. If anything feels off, we’ll tailor it in-session or via virtual coaching. Then, we’ll layer simple lifestyle tweaks to reduce daily jaw load.
Follow this Rocabado-inspired sequence 1–2 times daily; move slowly, breathe nasally, and stay within a calm, pain-free range.
Step 1: Resting tongue posture—tip on the spot behind upper incisors; seal lips, teeth apart; nasal breathe for 6 slow, quiet breaths.
Step 2: Controlled open and close—keep tongue up, jaw on midline; 3–4 seconds each way, 6 smooth reps.
Step 3: Isometric holds—one finger gives gentle resistance: opening, closing, right, left; hold 5–6 seconds, breathe, repeat x6 each.
Step 4: Cervical axial elongation—tiny chin nod, then lengthen the back of your neck; 6 controlled reps, no shrugging.
Step 5: Scapular setting—float shoulders down and slightly back; hold 3 seconds, relax; 6 light reps while keeping neck long.
Step 6: Self-massage—trace the masseter and temporalis; use light, slow circles for 60–90 seconds per side, staying under 3/10 discomfort.
Step 7: Lateral control—tongue up, glide jaw a few millimetres right/left; keep teeth apart and motion smooth; 6 easy reps.
For expert progressions and coaching in downtown Toronto, explore our therapeutic exercise program
designed to pair with jaw care.
Daily habits that supercharge your TMJ recovery
Those exercises work even better when your day supports them—use this quick checklist to lower jaw load starting now.
- Support your lower jaw when yawning—two fingers under chin to limit wide opening.
- At rest, keep lips together, teeth apart, tongue on palate to unload joints.
- During flares, choose softer foods; cut portions small and skip tough, sticky textures.
- Alternate chewing sides each bite to share load and avoid one-side overuse.
- Apply gentle heat 5–10 minutes before exercises to relax muscles and improve glide.
- Practice nasal breathing with light tongue suction on the palate to stabilize the jaw.
- Set screen at eye level; use an external keyboard and sit tall with relaxed shoulders.
- Sleep on your side or back with a pillow that keeps your neck neutral.
- Limit all-day earbuds and cue yourself: no tooth contact unless chewing.
- If you grind at night, discuss a night guard; we’ll coordinate with your dentist.
TMJ recovery timelines and milestones
If a night guard is part of your plan, your progress still follows a clear pattern. Results vary, and we’ll watch the signals—use this table for typical timelines, on-track signs, and when to escalate.
Case type Typical timeline Visit frequency Home program dosage Signs you’re improving When to escalate
Mild myofascial TMD (muscle-dominant jaw pain) 3–6 weeks to settle and build control Weekly for 2–3 weeks, then biweekly taper Brief practice 6x/day: posture, controlled opening, isometrics Less morning stiffness; fewer tender spots; clicks less frequent Pain rises or spreads despite consistent program for 2 weeks
Disc displacement with reduction (clicking, motion preserved) 6–10 weeks to quiet the click and control Weekly early; taper as midline control improves 4–6x/day exercises with posture and breathing drills Click becomes quieter/controlled; opening tracks midline Locking episodes persist, worsen, or opening drops under 35 mm
TMJ arthralgia/arthritis (joint irritation or wear) 8–12+ weeks with flare-and-calm cycles Weekly sessions; flare management and gradual taper Daily mobility, isometrics, heat; chew graded portions Chewing tolerance increases; night pain and flares reduce Night pain, swelling, or warmth escalates despite care
Chronic complex (neck + jaw + stress pattern) 10–16+ weeks with steady, layered progress Weekly then biweekly; add coaching for sleep/stress Short daily blocks, recovery breaks, and habit resets Headache days drop; opening stays midline and smoother Dizziness, numbness, or other neurologic symptoms emerge
From daily clicks to confident chewing
We watch for red flags like dizziness or numbness, but most journeys are steadier. Take a 32-year-old downtown office pro: daily clicks on calls, morning tightness, and a low laptop. Findings: opening 31 mm (millimetres) with a left drift, loud early click, tender masseter and temporalis (chewing muscles), forward head posture, and mouth breathing. Plan: gentle jaw and neck manual therapy, tongue-up controlled opening, chin tucks, isometrics, ergonomic tweaks, heat, and the cue “lips together, teeth apart.” Week 2: pain eased from 6/10 to 3/10, opening 36 mm, click quieter; mornings softer. Week 6: opening 42 mm on midline, headaches dropped from 5 days to 1, chewing on both sides without guarding. Week 10: click faint and occasional, only with big yawns; visits tapered from weekly to monthly.
Food freedom returned gradually. In week 8 they tested a bagel; by week 10 they managed crisp apples and steak (small bites, alternating sides) without a flare over 2/10. Opening held at 42–44 mm, midline stayed smooth, and morning tightness faded. Workstation fixes and nasal breathing kept clenching low. We spaced visits to every 3–4 weeks with a simple flare plan: scale range, switch to isometrics, heat, breathe, reassess in 48–72 hours. Confident again. Wondering if you need a night guard, imaging, or virtual care? We cover those common questions next.
Your top TMJ questions—night guards, imaging, and more
Is jaw clicking always harmful?
Not necessarily. If the click is painless and you can open smoothly on the midline, we manage it with control and load—not force. Many people see clicking soften as tongue-up opening and gentle isometrics improve coordination. That’s progress. If the click hurts, the jaw starts to lock, or your opening drops under 35–40 mm, book an assessment. Pain or unpredictability changes the plan. Quiet, controllable clicks are usually manageable; painful or locking clicks deserve a closer look.
Do I need X-ray or MRI for TMJ pain?
Usually no. Most TMJ pain settles with education, exercise, and load changes without imaging. Get imaging sooner after trauma, fever/swelling suggesting infection, progressive numbness, or a true lock lasting 24–48 hours. It also helps when we suspect arthritis, a non‑reducing disc, or if six to eight weeks of good rehab brings no change. We’ll examine you first and decide together if X‑ray or MRI (magnetic resonance imaging) will actually change your treatment.
Can TMJ cause dizziness or ear fullness?
Yes—sometimes. The jaw and upper neck share nerve pathways, so tension can refer to the ear or feel like lightheadedness. First, rule out medical causes like ear infection or blood pressure issues. If you notice true spinning, imbalance, or persistent fullness with head movement, our vestibular physiotherapy
can assess inner-ear factors while we treat your jaw and neck. Quick check: if relaxing your jaw and posture eases it within minutes, it’s likely musculoskeletal.
Will a night guard fix everything?
A night guard can reduce grinding forces and protect teeth, but it won’t fix daytime clenching, posture, or neck mechanics by itself. The best results pair a properly fitted dentist-made splint with physiotherapy: tongue‑up control, isometrics, posture, and stress tools. We coordinate with your dentist to choose the right guard (hard/soft, upper/lower) and timing. Many people feel measurable relief within 2–3 weeks when both pieces run together.
Should I self-adjust or intentionally pop my jaw?
We don’t recommend it. Forcing a pop can irritate the joint or disc and teaches your nervous system to chase the click. Instead, use controlled tongue‑up opening, gentle isometrics, and a smaller, painless range during flares. If you feel stuck or start to lock, support the jaw with a hand, avoid wide yawns, and book an assessment—manual techniques plus exercise usually restore motion safely.
Ready to calm your jaw?
If you’re done chasing that pop and want a safe, guided plan, we’re here. Book a same-day TMJ assessment in downtown Toronto; we offer direct billing to most insurers. Most people feel a meaningful shift in 2–3 visits, with a clear home plan on day one.
Prefer a quick chat before booking? Call 416-975-0499 and we’ll map next steps in minutes. If you’re ready, use the button below—after-work slots and virtual visits make it easy.