End Shoulder Pain Fast: 3-Phase Recovery Plan | Toronto
John Velasquez • March 28, 2026
If Your Shoulder Still Hurts, Here's Why and What Works
You reach for the top shelf and feel that sharp jab, then rolling onto your side at night wakes you again. Or maybe it started after a pickup game and lingered through long laptop days. Whether it came on suddenly or crept in, you just want it gone. We get it. At Rosedale Wellness Centre, we map a simple 3-phase plan to calm pain, restore strength, and get you back to what you love - using natural, conservative care, not a handful of pills or a rush to surgery.
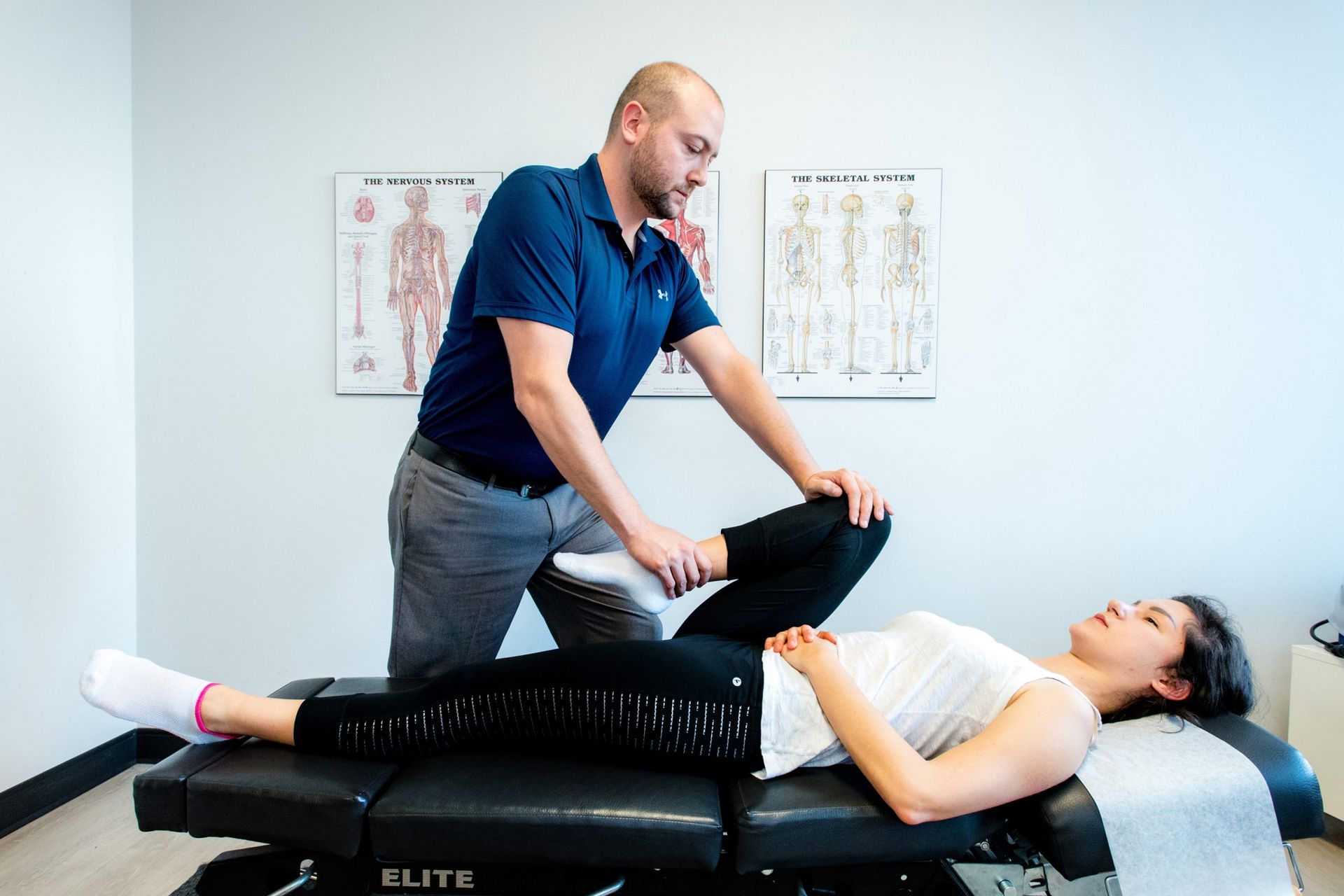
Your plan is personalized by a physio-led team: physiotherapy, chiropractic, massage, acupuncture, and laser therapy working together. We start with a thorough screen, rule out red flags, and only send you for imaging (X-ray, ultrasound, or MRI) when it truly changes care. Prefer a quick start? We offer same-day assessments in downtown Toronto, direct billing to most insurers, and evening or virtual visits. You’ll know exactly what to do between sessions, in 10–15 minutes a day, so pain settles, sleep improves, and lifting overhead stops feeling risky.
Next up: understand how this joint actually works, spot the true driver of your pain, and avoid common traps like chasing a 'perfect' scan. Then follow our step-by-step, 3-phase plan - with clear safety checks and professional guidance when you need it - so you can get back to moving confidently.
Your Shoulder: Big Motion, Bigger Coordination Demands
Before our 3-phase plan clicks, it helps to see the trade-off your shoulder lives with: tons of mobility if stability shows up. The rotator cuff (four deep muscles) and the labrum (a cartilage ring that deepens the socket) work like a camera gimbal—centering the ball while you move. Your shoulder blade’s control provides the platform so the arm can glide without friction. When those three coordinate, reaching, pressing, and throwing feel smooth. When they don’t, things get cranky. Fast.
Small losses of control create pinching or strain under everyday load. Picture a trailer hitch: if the ball isn’t lined up, every bump yanks the system. Same idea when you reach into the back seat, hoist a laptop bag, sleep with your arm overhead, or do push-ups with flared elbows. Add desk posture and a stiff upper back from laptop work, and the shoulder compensates—and complains. Tiny alignment errors become loud. Especially when repeated all week.
Your “shoulder” is really a team of four joints that must move together. If one falls behind, the others overwork. Meet the crew:
- Glenohumeral: main ball-and-socket for arm motion
- Scapulothoracic: shoulder blade gliding on rib cage
- Acromioclavicular: collarbone meeting the acromion
- Sternoclavicular: arm’s anchor point to the torso
Common Patterns Behind Shoulder Pain (And How They Present)
Most shoulder pain sits on a spectrum: overuse tendinopathies (irritated tendons), inflammatory bursitis (an inflamed cushioning sac), stiffness/frozen shoulder, and instability or trauma from a fall or sport. These layers often overlap—so a cuff ache can mingle with a pinchy arc from bursitis. That’s why symptoms blur and change day to day. Downtown routines—laptops, cycling with a heavy backpack, weekend gym sessions—add load to sensitive tissues. You’re not broken. You’re irritated, overloaded, and in need of guided rebuilding.
Diagnosis isn’t just a picture; it’s how your shoulder moves under load. Pain does not equal new damage—MRIs often show “tears” in people with zero pain, especially over 40. We prioritize functional findings—strength, control, range, and sleep tolerance—and reserve imaging for trauma, red flags, or stalled progress. If your pain is persistent or unclear, a focused assessment reveals the main driver and the safest starting point. Clarity lowers fear. And it speeds recovery.
Match your symptoms to a likely pattern below. Use these signature signs to narrow it down before we personalize your plan in clinic:
- Rotator cuff tendinopathy: ache on the outer shoulder, worse with lifting
- Impingement: sharp catch raising the arm overhead or reaching back
- Bursitis: diffuse ache with night pain and sore arc of motion
- Frozen shoulder: painful stiffness progressing to marked motion loss
- Instability/dislocation: sense of slipping, apprehension in certain positions
- Labral irritation/tear: deep click/catch after trauma or repetitive overhead sport
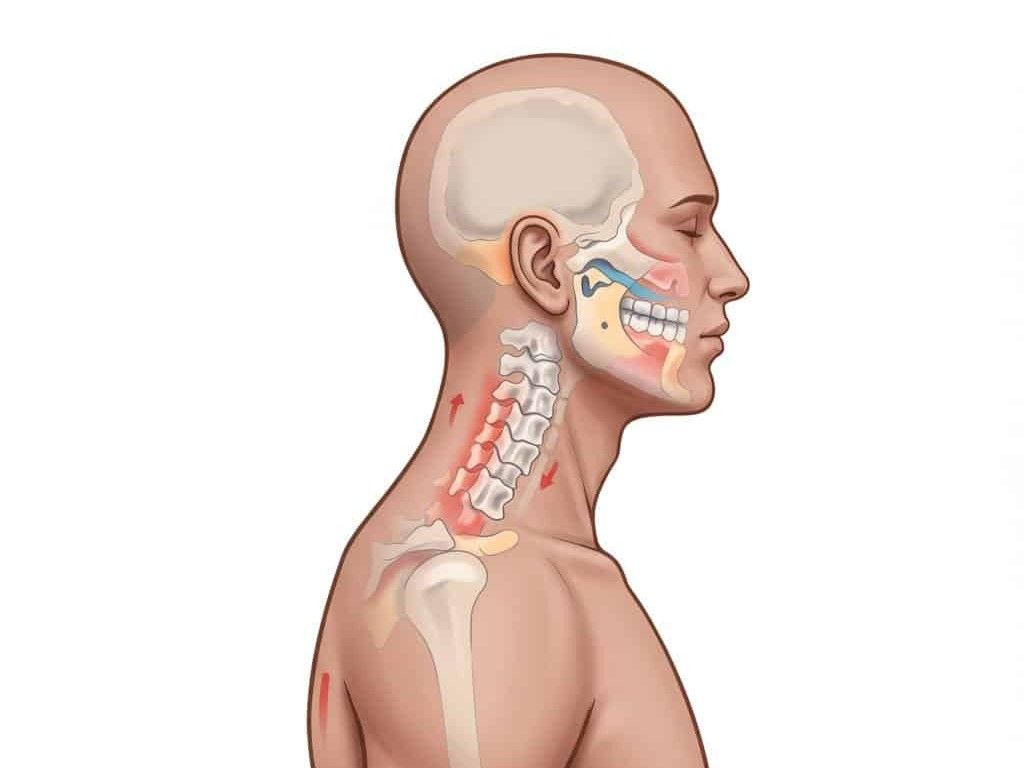
- Cervical referral: neck stiffness with tingling or pain radiating past the elbow
If your symptoms start in the neck or tingle past the elbow, see neck pain treatment Toronto
for next steps and relief options.
The 5 Mistakes That Prolong Shoulder Pain
These common missteps quietly add stress to irritated tissues and block healing. Notice how each either increases load or steals stability. Fixing them is often step one:
- Pushing through sharp overhead pain instead of modifying range
- Only resting—then returning to full load without rebuilding capacity
- Random online exercises without scapular control focus
- Skipping thoracic/neck mobility that supports the shoulder
- Ignoring sleep setup and workstation ergonomics
A Coordinated, Conservative Plan That Works
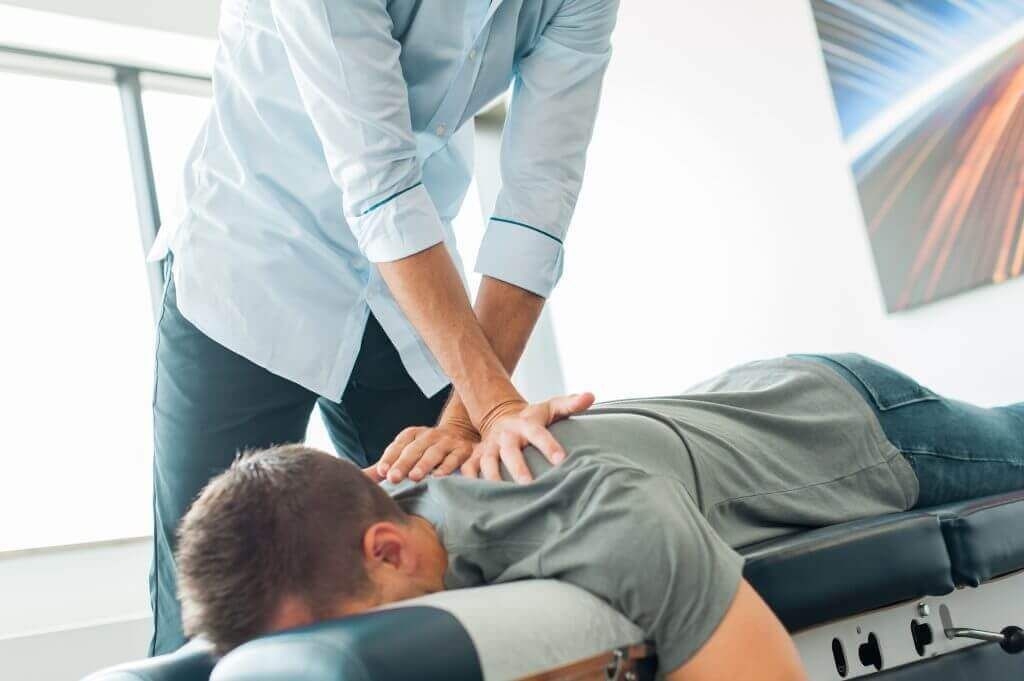
If those mistakes—like ignoring sleep setup or your workstation—rang true, our fix is coordinated and simple. We start with a thorough assessment of movement, load tolerance, shoulder-blade control, and neck/upper-back contribution, then dial in load management (what to ease, what to keep). Early focus is motor control and pain-calming strategies; we layer progressive strengthening as symptoms settle. Manual techniques and modalities—laser, acupuncture, taping—support the plan when needed. It’s easy to start: same-day appointments in downtown Toronto and direct billing to most insurers mean fewer hoops.
Your plan is personalized around your goals—sleeping through the night, lifting overhead, or returning to sport. We set clear metrics (pain scores, range of motion, strength benchmarks) and re-test every 2–3 weeks to keep progress visible. Your physio leads care and loops in chiropractic or massage when helpful, with notes shared so you never repeat your story. Expect practical timelines: many feel steadier sleep within 2–3 weeks and stronger reach by week 4–6. Same-day starts, direct billing, evening hours, and virtual rehab keep it convenient.
Start with physiotherapy Toronto—your coordinating hub for assessment, load management, and a tailored exercise plan. Your physio tracks metrics, adjusts weekly, and coordinates other services so each visit builds toward pain relief, better sleep, and confident overhead motion.
Stiff or guarded? manual therapy Toronto
uses joint and soft-tissue techniques to restore motion and ease protective spasm, so exercises land better. It’s an adjunct—not a standalone—and can calm painful arcs within the first few visits.
Add massage therapy downtown Toronto
for targeted soft-tissue relief that reduces tone, improves circulation, and helps you tolerate exercise. It pairs well with scapular control work and can settle post-workout soreness so you keep momentum between sessions.
When trigger points or stubborn guarding hold you back, we may use dry needling Toronto.
It targets irritable spots to relax muscle quickly, often improving range so you can load the shoulder safely right after.
kinesio taping Toronto
offers short-term support: gentle posture cues, swelling control, and pain modulation during daily tasks. We use it to keep symptoms quieter while you rebuild strength and control—not as a crutch.
The backbone is therapeutic exercise downtown Toronto: scapular control, rotator cuff loading, and graded overhead work. You’ll get a 10–15 minute daily plan with clear pain rules and progressions that match your milestones.
To bridge clinic and real life, active rehab Toronto
turns gains into function—lifting luggage, carrying a backpack, or pressing at the gym—with criteria-based progressions and coaching on technique.
If your pain followed a fall or sport-specific injury, our sports injury treatment Toronto
pathway layers in return-to-sport testing, power and stability benchmarks, and equipment or technique tweaks—so you get back safely, not just quickly.
💡
Need a Guided Plan?
Book a same-day shoulder assessment—direct billing available. We’ll triage quickly, start your plan, and give you the first exercises so you sleep better and lift easier this week.
From Painful to Powerful: Your 3-Phase Plan
You’ll leave that first visit with a plan—so what happens next? We guide you through three phases: calm pain, rebuild control, then return to performance. Most spend 1–3 weeks in Phase 1, 3–8 in Phase 2, and 8–12+ consolidating. Consistency beats intensity. Small daily wins compound.
Here’s what each phase targets—your goals, key focus areas, and the signs you’re progressing.
- Phase 1: Settle pain and restore motion—gentle ROM, isometrics, manual care; aim for night pain reduction and smoother daily tasks
- Phase 2: Rebuild control and strength—scapular coordination, rotator cuff loading; aim for pain-free range under light resistance
- Phase 3: Return to performance—task-specific loading, plyometrics as appropriate; aim for confident overhead work or sport skills
Match Your Symptoms to Smart Next Steps
Before you charge into Phase 3, map your symptoms to a likely pattern. Which row sounds like your shoulder? Find it, try the safe steps 7–10 days, and note help triggers. If things stall or worsen, we’ll guide you.
Condition Classic signs Try this at home (first 7–10 days) When to get help Typical recovery
Rotator cuff tendinopathy Outer upper-arm ache; worse with lifting, reaching, or side sleep Relative rest; cuff isometrics 20–30s holds; light heat Pain above 7/10 or night pain persists after a week Typically 6–12 weeks with guided loading
Impingement (subacromial pain syndrome) Sharp catch overhead or reaching into the back seat; painful arc Scapular setting; wall slides in pain-free arcs; posture breaks Catching pain doesn’t improve within 10 days Usually 6–10 weeks with progressive loading
Bursitis (inflamed cushioning sac) Diffuse ache, sore mid-range arc, night pain when rolling Ice 10–15 minutes, 2–3 times/day; gentle pendulums Marked weakness, visible swelling, heat/redness, or fever Often 4–8 weeks for acute cases
Frozen shoulder (adhesive capsulitis) Painful stiffness progressing to marked loss of motion Heat, gentle assisted range-of-motion, short holds; patience Rapid motion loss; diabetes or thyroid disease; sleep-ruining pain Typically 6–24 months; steady progress with guidance
Instability or dislocation Sense of slipping or dead arm; apprehension; often after trauma Sling briefly as advised; gentle pain-free range only First-time dislocation: go to the emergency room promptly Variable; 8–16+ weeks rehab; bracing or surgery if recurrent
Labral irritation or tear (cartilage rim injury) Deep click or catch after trauma or repetitive overhead sport Posture care; isometrics; avoid extreme ranges; technique checks Locking, repeated catching, or instability despite careful loading Usually 8–16+ weeks; longer for high-demand sport
Cervical referral (neck-related shoulder pain) Neck stiffness with pain or tingling past the elbow Neck mobility drills, chin nods, frequent position changes Numbness or weakness spreading into the hand; worsening night pain Often 4–12 weeks with combined neck and shoulder care
A Gentle Starter Routine (Pain-Free Range Only)
If your matrix row pointed to combined neck-and-shoulder care over 4–12 weeks, this gentle routine helps you start safely today. Work in a comfortable range (0–3/10 pain), slow tempo, and smooth control. Stop if pain sharpens, catches, or lingers after. Aim for 10–15 minutes total.
We’ll keep it gradual—small wins daily beat heroic sessions. AAROM means active-assist range of motion (you help the arm with a stick). ER/IR means external/internal rotation at your side. If you have diabetes, recent trauma, or night pain above 7/10, book a consult so we tailor safely. Most people notice easier sleep or reaching within 7–10 days with consistency.
Start with easy mobility, then light activation. Here’s your 10–15 minute circuit.
Step 1: Pendulums—2–3 minutes each direction; fully relax shoulder
Step 2: Scapular retraction/depression—2x10 slow reps against light band
Step 3: Supported flexion AAROM with stick—2x10 in pain-free arc
Step 4: Isometric ER/IR at the side—5x10–20s holds, gentle effort
Step 5: Wall slides with serratus reach—2x8, smooth control
For best results, we individualize reps, tempo, and progressions through therapeutic exercise downtown Toronto. A quick check-in lets us fine-tune loads to your goals, sport, and workspace so each week builds on the last.
Do This, Not That (While Your Shoulder Heals)
That 10–15 minute routine works best when your day supports it. We recommend these wins today—pillow support at night and posture timers during work.
- Do: Use pain-free arcs for tasks to avoid re-irritation
- Do: Take posture breaks every 30–45 minutes
- Do: Prioritize side-sleeping on the non-painful side with pillow support
- Do: Use ice for hot, irritable pain; heat for stiffness
- Do: Track 2–3 daily pain/function metrics to see progress
Now avoid habits that re‑irritate tissue and stall progress. Each adds load or steals stability. If pain spikes or red flags appear, see next section.
- Don’t: Push through sharp catching pain overhead
- Don’t: Jump back to full training after resting
- Don’t: Ignore neck/thoracic stiffness influencing the shoulder
- Don’t: Sleep directly on the painful shoulder
- Don’t: Rely solely on painkillers without a plan
Know the Red Flags (Don’t Wait)
If painkillers aren’t a plan and home tips aren’t enough, seek urgent care or book an assessment if any of these happen. We’ll triage same-day.
- Red flag: New deformity after trauma—go to ER
- Red flag: Arm/hand numbness or weakness—urgent medical review
- Red flag: Severe night pain unrelieved by rest—clinic assessment
- Red flag: Fever, redness, or warmth—rule out infection
- Red flag: Sudden loss of motion without reason—professional exam
- Red flag: Repeated dislocations or feelings of giving way—guided stabilization
From Night Pain to Overhead Strength in 12 Weeks
Once we ruled out those red flags, a 38-year-old downtown marketer came in with classic impingement: sharp overhead catch and 7/10 night pain. Assessment showed scapular dyskinesis (shoulder blade not tracking well) and rotator cuff irritability (tendon sensitive to load). We set load limits, used manual therapy (hands-on joint/soft-tissue work), taping for short-term support, and a targeted exercise plan. Results: by week 4, night pain 7→3/10; by week 8, flexion 130°→165°; by week 12, external rotation strength up 30% and overhead reach smooth.
We adjusted every two weeks. Phase 1 focused on pain-calming and isometrics (muscle holds) with pillow support and desk tweaks; a brief flare after moving day settled when we cut volume 30%. Phase 2 added scapular control progressions, cuff eccentrics (slow-lowering work), and light landmine pressing instead of overhead. By Phase 3, we layered thoracic mobility and return-to-gym coaching; massage eased post-session tightness, and one virtual check-in kept adherence high during travel.
Week 12 outcomes: pain 1–2/10, full flexion to 170°, external rotation strength +35%, and uninterrupted sleep. He lifted a carry-on overhead, resumed classes with modified presses, and stopped fearing that sharp catch. The lesson for you: consistent 10–15 minute work, smart loading, and a team that adjusts quickly beat rest alone. Curious about referrals, imaging, or billing? Our FAQs below clear the last hurdles so you can start confidently.
Your Questions, Answered
You asked about imaging, referrals, and billing—here are clear answers. If your situation is unique, bring your questions to your assessment and we’ll tailor the plan to you.
Q: Do I need an MRI right away? A: Usually no—try guided conservative care first unless red flags
Q: How long until I can sleep normally? A: Often 2–6 weeks with pain-calming and support
Q: Can I keep training? A: Yes—modify volume, range, and movements that catch
Q: Heat or ice? A: Ice for hot irritation; heat for stiffness
Q: When is surgery considered? A: Only if structured rehab stalls or instability is severe
Q: Best posture? A: The next one—move often; build endurance, not rigid positions
Q: Will taping or needling fix it? A: They help tolerance; progressive loading drives lasting change
Ready for Relief? Start Today
Lasting change comes from progressive loading—so let’s build your plan now. Book a same-day assessment in downtown Toronto, with direct billing to most insurers and a physio-led team coordinating chiropractic, massage, acupuncture, and laser as needed. We tailor care to your life, from sleeping without pain to pressing overhead or returning to rec league. You’ll leave visit one with clear exercises and pain rules.
Prefer low-friction access? Book online in under two minutes, choose evening or virtual visits, and start Phase 1 today. Many people notice easier sleep within 2–3 weeks and smoother reach by weeks 4–6 with a 10–15 minute plan. We’ll track pain, range, and strength so you see progress—not guess.
Start your shoulder pain relief Toronto
journey now—same-day assessments, direct billing, and evening or virtual options.
Why Choose Rosedale Wellness Centre
Book your assessment with confidence—here’s why we’re trusted. Your care is delivered by licensed physiotherapists, chiropractors, registered massage therapists, and acupuncturists working together under one roof. Recognized among the city’s top wellness clinics, we make starting easy: same-day appointments, evening spots, and direct billing to most insurers. You’ll leave visit one with a clear plan and support between sessions. Prefer in person? Find us at 120 Bloor St E with TTC (Toronto’s subway) access nearby. Want to talk first? Call 416-975-0499 and we’ll match you with the right clinician for your goals.
How will you know it’s working? We set measurable goals—pain, range of motion, strength, and sleep—and re-test every 2–3 weeks. Your physio leads care and loops in chiropractic, massage, or acupuncture as needed so each visit builds on the last. Most people notice night pain easing within 2–3 weeks and smoother overhead reach by weeks 4–6 when they follow the plan. Booking is simple: call 416-975-0499 or schedule online in under two minutes. Need flexibility? Choose evening appointments or virtual rehab. Direct billing keeps costs predictable, so you can focus on getting better.