Neck Pain Treatment: Fast Relief & Expert Exercises
John Velasquez • March 28, 2026
Neck Pain: Causes, Symptoms, Treatment and Exercises
Why your neck hurts isn’t just “bad posture”
Causes, symptoms, treatments, exercises—all helpful, but they miss one truth: your neck reacts to what you ask of it and how you recover. After a 10-hour laptop marathon at a hot desk, it tightens by dinner. Then you doom-scroll at 2 a.m., sleep crooked, and wake with a concrete neck. It’s not just posture. It’s load, recovery, and habits stacking up.
Think of it like a volume dial: stress, poor sleep, and long holds turn sensitivity up—even when nothing is newly “damaged.” On a rested day, the same desk setup feels fine; after a crunch week, a five-minute email flares it. We see this daily at Rosedale. Small, frequent movement and steady strength work turn that volume down.
So where does this show up in your day? Let’s spot the patterns—work setup, TTC (Toronto Transit Commission) commutes, weekend workouts, and sleep—and give you quick wins you can try today. Ignore it and it lingers; address the drivers and you can feel change within days.
How neck pain sneaks into everyday life
You asked where this shows up in your day—it’s the mix of long sitting, hybrid work, and multi-screen setups that quietly stack load on a sensitive neck. Laptop low, phone high, shoulders creeping up during calls. Movement drops, stress lifts baseline muscle tone, and sleep position finishes the job. It’s rarely one “bad posture.” It’s cumulative load and a sensitized system that needs smart breaks and better support.
Real life multiplies it: hot-desking without a stand, reading on the TTC (Toronto Transit Commission) with your chin tucked, cycling with bars too far, or hauling a one-strap bag. New parents cradle on one side; weekend warriors hammer overhead presses after a desk week; jaw clenching during crunch time locks the upper neck. The fix isn’t heroic. With a few guided tweaks and the right exercises, we reduce friction so your day asks less of your neck while you build capacity.
Left alone, neck pain chips away at work focus, sleep quality, workouts, and mood. Spotting your pattern is the first lever. In the next section, match your symptoms to common profiles so we can target the right plan for you.
Symptoms decoded: what your neck pain is telling you
Here’s a quick tour of symptom patterns. Find the one that sounds like you, then we’ll tailor next steps. If you’re not sure, just note what changes with movement versus rest.
- Neck ache with stiffness after screens; better with movement.
- Sharp “catch” turning head on waking; motion blocked to one side.
- Headache starting at base of skull, wrapping to forehead or eye.
- Burning/tingling down shoulder/arm with certain neck positions.
- Dizziness/imbalance accompanying neck pain, especially after injury.
⚠️ Urgent symptoms—seek medical care now
Call 911 or go to urgent care if you have: recent severe trauma; progressive weakness or numbness in an arm or hand; loss of coordination or trouble walking; fever or feeling unwell with neck stiffness; unexplained weight loss or a history of cancer; a sudden, severe “worst-ever” headache; or new bowel or bladder changes. These can signal something more serious than mechanical neck pain. Don’t wait—seek medical attention now. If you’re unsure, call us and we’ll help you triage the next best step.
The good news: most neck pain is mechanical (irritated joints and muscles, not structural damage) and improves with conservative care. The key is matching treatment to your pattern—education, manual therapy, and the right exercises—rather than a one-size plan. We’ll show you how we do that.
Why quick fixes fail: the hidden drivers of recurring neck pain
Quick fixes fade because several drivers pile on at once. If we don’t address them together, relief doesn’t stick. These are the usual suspects we test.
- Underloaded deep neck flexors and scapular stabilizers.
- Overreliance on passive care without progressing to strength.
- Ergonomic friction: laptop heights, screen distance, chair arms.
- Sleep position and pillow mismatch maintaining joint/muscle tension.
- Stress, jaw clenching, and breath-holding elevating tone.
- Confidence fears leading to activity avoidance and deconditioning.
Lasting relief comes from a plan that calms pain, restores motion, and then loads the system progressively while removing daily triggers. That’s exactly how our multidisciplinary care works—let’s map your week-by-week path next.
The Rosedale plan for lasting relief
You just saw that lasting relief comes from calming pain, restoring motion, then loading smartly. We follow that arc: calm, restore, rebuild, and bulletproof your habits—with a plan tailored to your day. Start same day, use direct billing, and leave visit one with clear steps and targets. Most feel change in 3–7 days.
We coordinate four pillars that move you from flare to resilient.
- Assessment and education: precise diagnosis, aggravator mapping, goal-setting; reassure and set expectations.
- Pain relief and mobility: targeted hands-on care, gentle movement, and modalities as needed to settle symptoms.
- Strength and control: progressive deep neck flexor, scapular, and postural loading tailored to capacity.
- Habit and environment reset: practical workstation, sleep, and activity tweaks that fit real life.
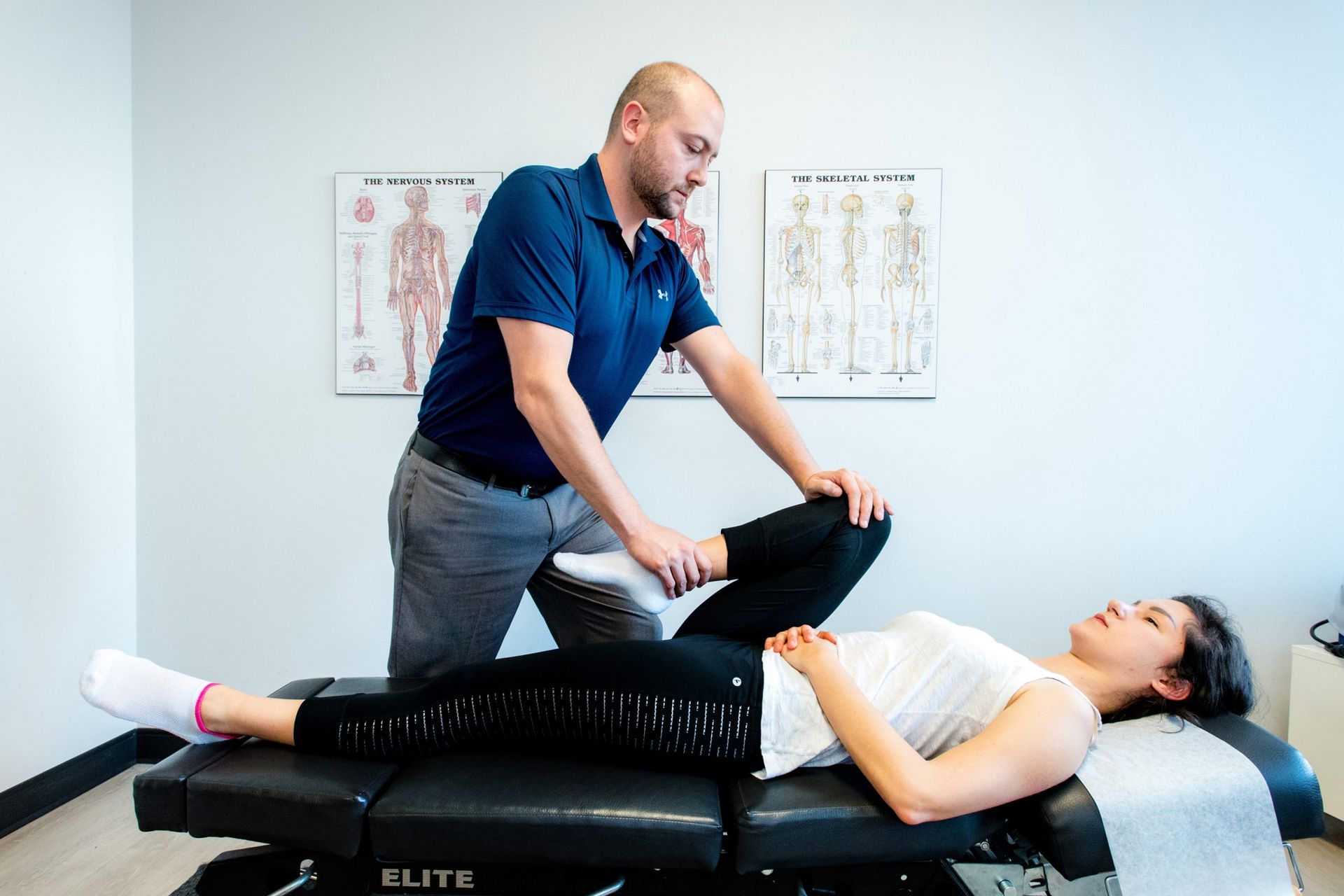
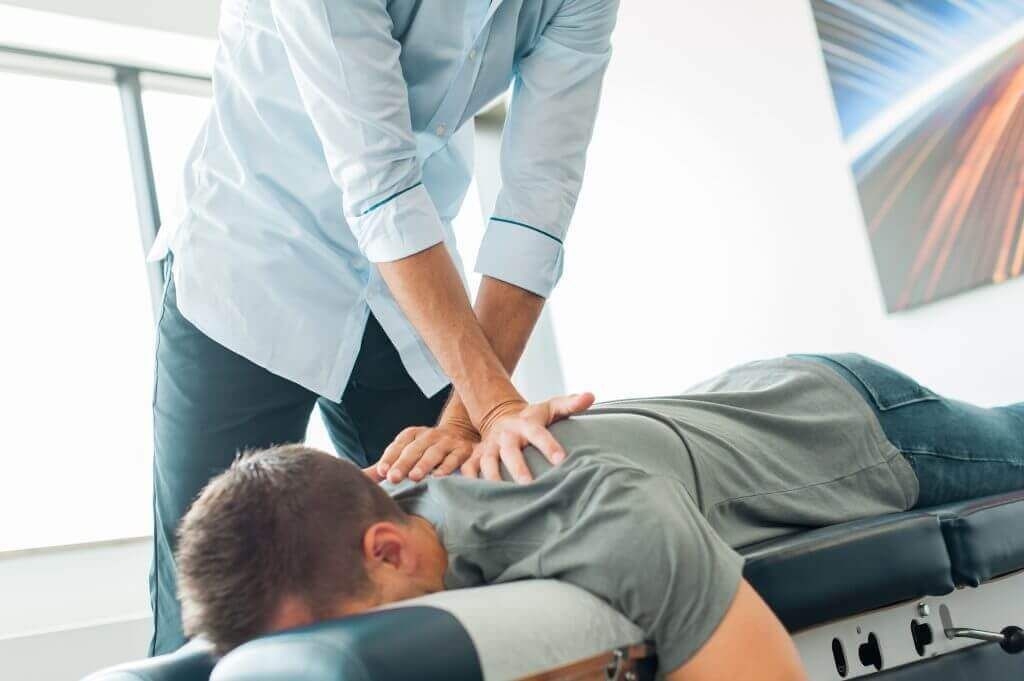
Hands-on care can quickly lower sensitivity and free up movement so exercises work better. When appropriate, we use manual therapy
to mobilize stiff joints and ease tight tissue—always paired with active rehab, not as a standalone fix.
Acupuncture or dry needling (precise, thin needles), massage, laser, or taping can help calm pain and muscle tone in early phases. We use them selectively, based on your response, while progress is measured by motion, sleep, and daily function. Next, we’ll map your week-by-week progression.
What treatment looks like, week by week
Phase Primary focus In-clinic care At-home plan Progress markers
Week 0–1 Calm irritation and restore gentle motion; find positions of relief and reduce sensitivity We apply targeted joint and soft‑tissue techniques; acupuncture or laser if helpful; coach safe movements You’ll do little‑and‑often pain‑free range of motion; 5–10 minute walks; heat or ice as comfortable; brief breathing drills Pain settles 20–30%; turning improves; sleep slightly better; less guarding with head checks
Weeks 1–3 Rebuild mobility and control; begin endurance in deep neck flexors and scapular support We guide mobility, motor‑control drills, and technique; progress isometrics; refine ergonomics for desk, commute, and sleep You’ll do daily range of motion; 3–5 sets of chin nods; light band rows/face pulls; 30–30 breaks; 10–15 minute walks Rotation reaches shoulder line; side‑bend smoother; fewer flare‑ups; sitting tolerance up by 30–60 minutes
Weeks 3–6 Strengthen and build tolerance; progress endurance and integrate whole‑body support We progress loading for neck and scapula; conditioning circuits; practice job/sport tasks; introduce heavier carries or pulls You’ll run a 3x/week strength routine: rows, pulldowns, face pulls; longer walks or cycling; refine workstation; graded return to gym/sport Work and workouts last longer; confidence up; minimal morning stiffness; chin‑tuck hold 20–30 seconds without strain
Week 6+ Resilience and prevention; prepare for high‑demand weeks We run higher‑load progressions; refine sport/work‑specific skills; finalize relapse‑prevention plan and self‑testing checklist You’ll maintain strength 2–3x/week; mobility on active days; cardio; stress and sleep strategies; taper visits as you self‑manage Feels normal; rare, short flares with quick recovery; confident self‑management; ready for peak workloads or sport
Your safe home plan: 24 hours to 4 weeks
To lock in that “feels normal” momentum, use this home plan alongside your visits. Progress only if discomfort eases within 24 hours; back off 30–50% if symptoms spike.
Step 1: Settle pain | 10–15 minutes of heat or ice as tolerated, 2–3x/day.
Step 2: Gentle motion | Little-and-often ROM: rotation, side-bend, nodding within comfort.
Step 3: Micro-breaks | 30–45 minute posture breaks; stand, walk, reset shoulders.
Step 4: Sleep setup | Try side-sleep with neutral neck; adjust pillow height.
Step 5: Medication | If needed, discuss OTC options with pharmacist/doctor; use short-term.
Step 6: Track triggers | Note positions/loads that flare symptoms to refine your plan.
Keep moving gently—reduce, not stop. If pain persists beyond 10–14 days, ramps up, or arm weakness/numbness appears, book an assessment; we’ll tailor exercises and progressions to get you back on track.
Best exercises for neck pain (and how to progress them)
You’re already moving gently—ready to turn that into targeted work? 10–15 minutes, 5–6 days a week beats marathons; if symptoms spike or shoot into your arm, scale back 30–50%.
- Chin nods: gentle deep neck flexor activation; progress to holds. Start supine, tiny nod as if saying yes; 2–3 sets of 8–10 reps, then holds 5–10 seconds, pain-free.
- Scapular retraction rows: band or cable; progress reps/load. Elbows by sides, squeeze shoulder blades down/back; 2–4 sets of 10–15, 3–4 days/week; add band tension when last 2 reps feel strong.
- Thoracic extension over towel: mobilize upper back; progress duration. Roll towel lengthwise, place mid-back, hands support head; 5–8 slow extensions, 2–3 sets; breathe out on the way back.
- Side-bend isometrics: light hand resistance; progress angles/time. Sit tall, ear to shoulder gently into hand; hold 5–10 seconds, 5–8 reps each side; try slight forward/backward angles as tolerated.
- Neck rotation AROM (active range of motion): small to larger arcs; progress speed/control. Turn toward shoulder within comfort; 10 slow reps each way, 2–3 sets; add end-range holds 3–5 seconds.
- Breathing drills: slow nasal inhale, long exhale; progress to standing. 4–6 in, 6–8 out; 2–3 minutes before bed or after desk blocks; then stand with relaxed jaw and shoulders.
Want a custom video plan and form coaching matched to your capacity? Explore therapeutic exercise
with our team—we’ll tailor progressions and variations for headaches, jaw (TMJ, temporomandibular joint), or dizziness next.
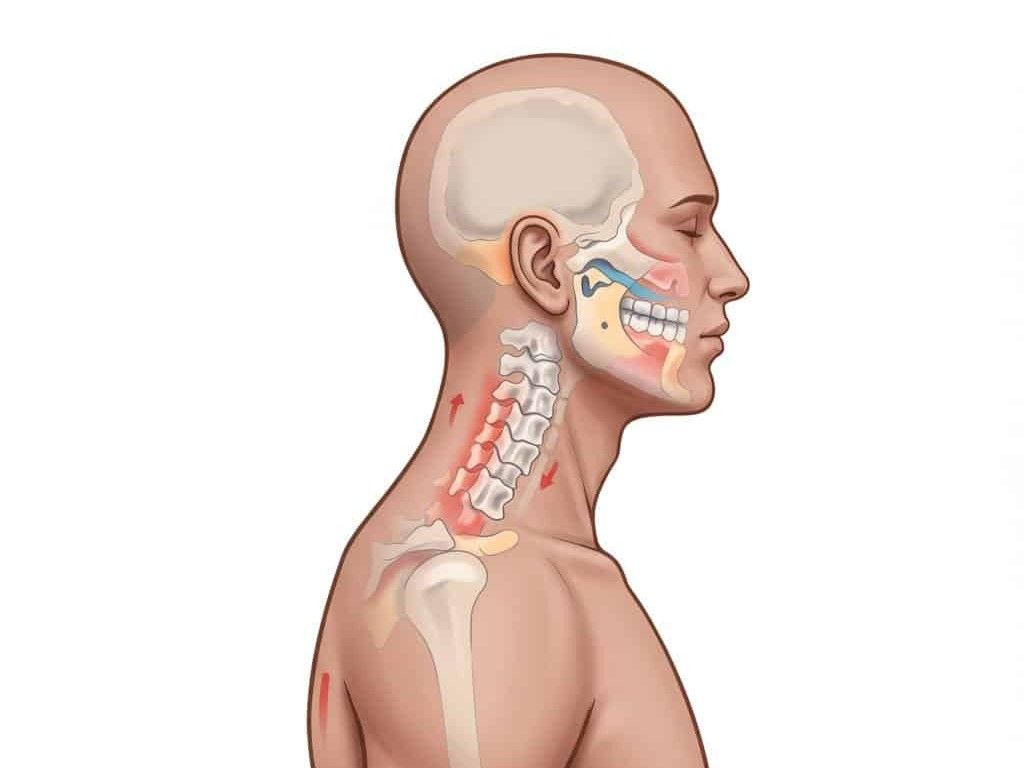
Headaches, jaw (TMJ), and dizziness: when neck pain isn’t just the neck
As promised, when headaches, jaw, or dizziness show up, we treat the neck and the system it talks to. Cervicogenic headache means neck joints/soft tissue refer pain to the head (often base-of-skull to eye). TMJ (temporomandibular joint)-related neck pain pairs clenching or popping with upper-neck tension. Cervicogenic dizziness is neck-driven imbalance; vestibular causes come from inner ear or concussion. Management blends neck rehab plus jaw/vestibular care as needed.
Jaw clicking, morning soreness, or clenching? Book an assessment and we’ll pair neck rehab with bite and habit coaching. Learn how we treat it on our TMJ dysfunction treatment
page—co-managed with dental partners when needed.
Dizzy with neck turns, or off-balance after a concussion? We’ll test neck and inner ear. If needed, we coordinate vestibular physiotherapy
alongside cervical rehab so you regain steadiness in days to weeks.
Headache tip: Two minutes of suboccipital release (tennis balls at skull base) plus 5 breath cycles (inhale 4–6, exhale 6–8) before screens. Then 10 chin nods. It often reduces ache; we’ll map timelines next.
How long recovery takes—and what good progress looks like
As promised after those headache tips, let’s map timelines. Recovery varies by cause and consistency; with a solid plan, here are the ranges most Toronto desk-workers see.
- Muscle strain: 2–6 weeks with consistent loading and sleep fixes.
- Wry neck/joint lock: 1–3 weeks once motion is restored early.
- Radiculopathy: 6–12+ weeks; steady nerve symptom retreat is key.
- DDD/arthritis: ongoing management; strength and habits reduce flares.
If you’re not improving by weeks 2–3, or you notice worsening numbness, weakness, or growing limits in work or sleep, we escalate. We’ll re-assess, coordinate imaging or specialist referral, and adjust your plan—no delays.
A real-world story: From desk-bound pain to confident movement
We escalate fast if week 2–3 stalls; when it doesn’t, progress looks like this. A mid‑30s professional near Yonge–Bloor came in with 7/10 neck pain, rotation stuck at 40° left, waking 3x/night, and arm tingling at the laptop. Same‑day assessment: irritated facet joints, tight suboccipitals, deep neck flexor endurance 5 seconds; neuro screen normal. We started manual therapy, laser for pain modulation, gentle ROM, chin nods, and quick desk tweaks. By day 7: pain −30%, rotation +15°, sleep down to one wake‑up.
Week 2–3, we added acupuncture, progressed isometrics and band rows, and dialed in pillow height. Pain dropped 60%, sitting tolerance grew by 60 minutes, and rotation reached the shoulder line. By week 4, full rotation returned; cycling felt easy after a small handlebar reach change. Week 5, back to the gym with a graded plan. Week 6–7, chin‑tuck hold hit 30 seconds and two‑hour meetings were comfortable. They left with a relapse plan—and confidence. Ready to feel the same?
Ready to feel better? Your next steps
Ready to feel the same? Book online for a same-day assessment or call 416-975-0499. We offer direct billing and no referral needed, so getting started is easy. Not sure what’s going on? Start with an assessment and leave with a clear diagnosis, a pain-calming plan, and your home program.
Prefer a straightforward start? Our physiotherapy
team can assess, treat, and build your plan in one visit.
Want details on techniques, timelines, and exercises? Explore our neck pain treatment
guide to see how care progresses from week one to return-to-sport.